Why are hospitals still losing millions in denied claims even after investing heavily in claim scrubbing software?
Healthcare organizations today are under constant pressure to reduce claim denials, improve reimbursement cycles, and accelerate payer approvals. Yet many hospitals, clinics, and revenue cycle management companies continue to struggle with clean claim rates below 90%. Traditional claim scrubbers are no longer enough in a healthcare ecosystem driven by complex payer policies, evolving compliance regulations, and AI-assisted fraud detection systems.
This is where AI claim scrubber management software development becomes a strategic investment instead of just another operational upgrade. Healthcare enterprises are now exploring smarter solutions that can predict denial patterns, automate coding validation, detect payer-specific issues, and improve first pass claim acceptance rates before claims are submitted.
The demand for developing AI claim scrubbing platform for insurance and hospital revenue cycle management is increasing rapidly. According to Precedence Research, the AI for healthcare payer market surpassed USD 5.70 billion in 2025 and is projected to reach nearly USD 46.67 billion by 2035, growing at a CAGR of 23.40%.
Healthcare CIOs, hospital administrators, insurance providers, RCM companies, healthtech startups, and digital healthcare investors are actively searching for ways to develop smart claim scrubber workflow automation software that reduces denials and maximizes reimbursements.
Many organizations are now asking an important question:
“I am planning to build an AI-powered claim scrubber software for hospitals. Which healthcare software development company can help us?”
The answer depends on choosing a technology partner with deep expertise in healthcare compliance, AI automation, interoperability standards, predictive analytics, and scalable cloud-native healthcare architecture. More importantly, the right partner must understand how to create an AI claim scrubber tool that improves first pass claim acceptance rates while maintaining HIPAA compliance and payer rule accuracy.
AI Claim Scrubber Management Software is an intelligent healthcare billing solution that automatically checks medical claims for errors, missing information, coding issues, and payer-specific compliance problems before claim submission. The primary goal of this software is to improve clean claim rates, reduce claim denials, and accelerate insurance reimbursements.
Unlike traditional rule-based systems, AI-powered claim scrubbers use machine learning, predictive analytics, and workflow automation to identify hidden claim risks and continuously improve claim accuracy over time. This makes AI claim scrubber management software development a growing priority for hospitals, insurance providers, and revenue cycle management companies.
Organizations investing in developing AI claim scrubbing platform for insurance workflows can significantly reduce manual billing efforts and improve first pass claim acceptance rates.
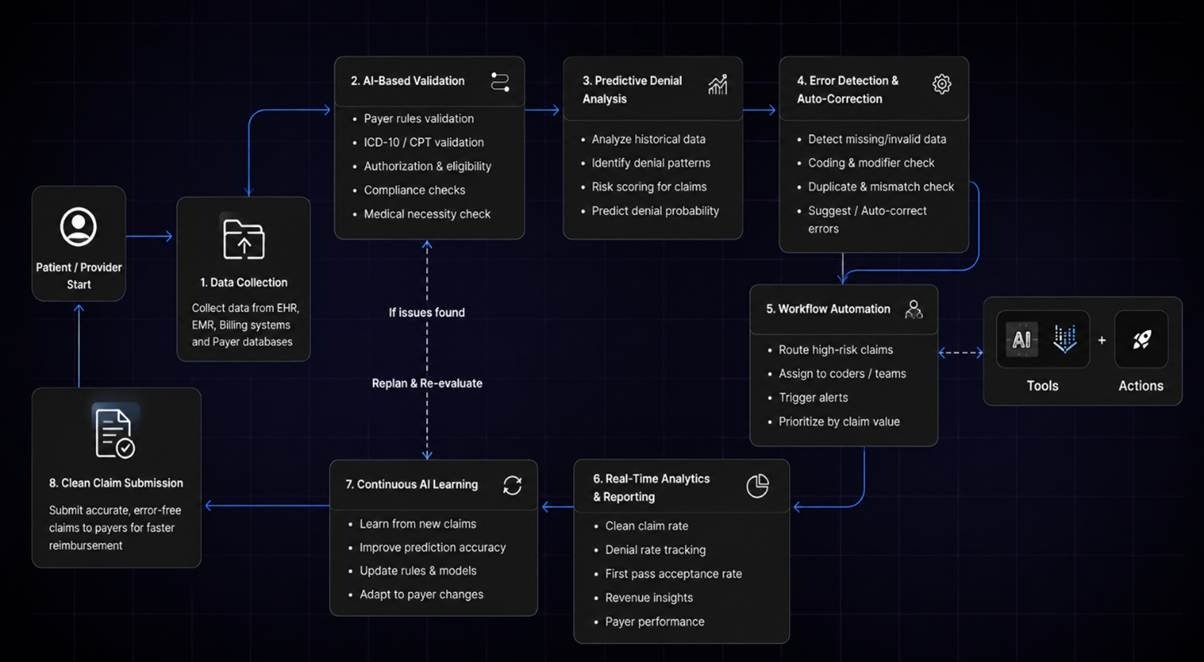
The software connects with EHRs, EMRs, billing platforms, and hospital databases to collect patient records, diagnosis codes, insurance details, and treatment information in real time.
The AI engine checks claims against payer rules, ICD-10 and CPT coding standards, authorization requirements, and compliance guidelines to identify possible errors before submission.
Machine learning algorithms analyze past denied claims and payer behavior to predict which claims are most likely to be rejected.
The platform detects missing modifiers, duplicate billing entries, incorrect coding combinations, and incomplete documentation. Advanced systems can also suggest corrections automatically.
Claims with high-risk issues are automatically routed to coders, billing teams, or compliance managers for review, reducing manual workload and processing delays.
The software provides dashboards that track denial rates, clean claim percentages, reimbursement trends, and overall revenue cycle performance.
The AI model continuously learns from new claims, payer responses, and denial outcomes to improve prediction accuracy and claim validation performance over time.
By helping healthcare organizations develop smart claim scrubber workflow automation software, AI-driven platforms improve operational efficiency, reduce claim rework, and maximize reimbursement success.
Also Read: AI Claim Denial Management Software Development
Many healthcare organizations believe that simply implementing a claim scrubbing tool will automatically reduce denials and improve reimbursements. However, the reality is very different. Most hospitals, clinics, and revenue cycle management providers still struggle to maintain clean claim rates above 90% because traditional systems cannot keep up with the growing complexity of modern healthcare billing.
As payer policies become stricter and compliance requirements continue evolving, outdated claim scrubbing systems create operational bottlenecks instead of solving them. This is one of the biggest reasons why AI claim scrubber management software development is becoming essential for healthcare organizations aiming to improve revenue cycle performance.
According to KFF Research Report, insurers denied nearly 20% of healthcare claims was in 2024 for ACA marketplace plans. This means almost 1 out of every 5 submitted claims faced rejection or payment delays.
In another industry report, Experian Health State of Claims Survey found that 41% of healthcare providers experienced denial rates of 10% or higher due to outdated workflows, staffing shortages, and claim data errors.
These numbers clearly show why healthcare enterprises are now prioritizing developing AI claim scrubbing platform for insurance and hospital billing automation.
Most traditional claim scrubbers rely on static rule engines that only detect predefined claim errors. These systems cannot learn from denial history or predict future claim risks.
As payer rules evolve, static systems become less effective, resulting in repeated denials and costly claim rework.
Healthcare organizations that develop smart claim scrubber workflow automation software with AI capabilities gain a major advantage because AI continuously adapts to payer behavior and denial trends.
Insurance companies frequently update:
Traditional scrubbers often fail to update fast enough, causing claims to violate the latest payer requirements.
This creates a major gap between claim submission and payer expectations.
Most existing claim scrubbing systems work reactively instead of proactively.
They identify errors only after claims are generated rather than predicting denial probability before submission.
Modern AI claim scrubber management software uses machine learning models to analyze:
This predictive capability significantly improves first pass claim acceptance rates.
According to Health Catalyst Research, nearly 86% of healthcare claim denials are potentially avoidable with better predictive technologies and workflow automation.
Many healthcare organizations still operate disconnected systems across:
Poor integration creates:
Without seamless interoperability, claim accuracy suffers significantly.
Medical coding remains one of the leading causes of claim denials.
Human coders may unintentionally submit:
AI-powered coding validation engines help detect these issues instantly and improve coding accuracy across departments.
Manual claim review workflows slow down reimbursement cycles and increase administrative costs.
Billing teams often spend hours correcting preventable claim errors manually.
Organizations that invest in AI claim scrubber management software development can automate:
This drastically improves operational efficiency.
Traditional claim scrubbers provide very limited reporting capabilities.
Healthcare organizations often lack visibility into:
Without advanced analytics, revenue cycle teams cannot make proactive improvements.
Modern AI-powered dashboards provide real-time insights that help healthcare leaders optimize financial performance continuously.
Healthcare compliance regulations continue evolving rapidly.
Organizations must constantly align with:
Managing these requirements manually becomes extremely difficult at scale.
According to Premier Healthcare Report, healthcare providers spend billions annually managing claim adjudication and denial-related administrative processes, much of which can be reduced through intelligent automation.
The healthcare reimbursement landscape is becoming more complex every year. Payers are increasingly using AI-assisted claim reviews, stricter fraud detection systems, and advanced denial management algorithms.
This means healthcare providers can no longer rely on outdated claim scrubbing systems.
Organizations exploring how to create an AI claim scrubber tool that improves first pass claim acceptance rates are now focusing on intelligent automation, predictive analytics, and real-time payer intelligence to stay financially competitive.
AI-powered claim scrubber platforms are no longer optional. They are becoming a core technology requirement for modern healthcare revenue cycle management.
So, these are the major reasons why many healthcare organizations still struggle with low clean claim rates despite using traditional claim scrubbing systems.
Traditional claim scrubbers mainly work as static rule-checking systems that detect billing mistakes after claims are created. AI-powered claim scrubber management software operates very differently. It acts as an intelligent revenue cycle engine that predicts, prevents, and resolves claim issues before submission.
This is one of the biggest reasons why healthcare organizations are increasingly investing in AI claim scrubber management software development to improve clean claim rates, reduce denials, and automate complex claims workflows.
Modern AI-powered platforms continuously analyze payer behavior, historical denials, coding trends, clinical documentation, and reimbursement outcomes to optimize every stage of the claims process.

Traditional scrubbers validate claims sequentially, which slows down workflows and often misses cross-checking opportunities between payer policies and coding rules.
AI-powered claim scrubbers validate claims in under 3 seconds against NCCI edits, LCD/NCD policies, MUE limits, authorization requirements, compliance standards, and payer-specific reimbursement rules simultaneously. This real-time validation process helps healthcare organizations dramatically improve first pass claim acceptance rates while reducing manual intervention.
One of the most advanced capabilities of developing AI claim scrubbing platform for insurance workflows is Natural Language Processing (NLP).
Instead of reviewing documentation after claim submission, AI systems analyze physician notes, treatment summaries, patient encounters, and clinical records before claims are coded. The platform automatically identifies missing medical necessity details, unsupported procedures, incomplete documentation, and coding inconsistencies that could trigger denials later in the revenue cycle.
This proactive approach significantly reduces preventable claim rejections.
Traditional claim scrubbers require manual rule updates every time payer policies change.
AI claim scrubber management software continuously learns from historical denials, reimbursement outcomes, claim approvals, coding corrections, and payer adjudication behaviors. The more claims the system processes, the more accurate and intelligent it becomes.
This adaptive learning capability makes AI-powered platforms far more effective than static rule-based systems and is one of the key advantages of develop smart claim scrubber workflow automation software.
Conventional scrubbers typically stop after flagging errors, leaving billing teams responsible for manually researching fixes.
AI-powered systems go beyond detection by recommending the correct diagnosis codes, modifiers, missing billing elements, and payer-specific adjustments automatically. Billing staff can resolve issues instantly without wasting time on repetitive manual reviews.
This not only improves efficiency but also accelerates reimbursement cycles.
Modern AI claim scrubber management software assigns a denial probability score to every claim before submission.
High-risk claims are automatically flagged for review, while low-risk claims move through the workflow without unnecessary delays. This intelligent prioritization helps healthcare organizations focus human attention only where it delivers the highest value.
Healthcare enterprises exploring how to create an AI claim scrubber tool that improves first pass claim acceptance rates heavily depend on predictive denial scoring to optimize operational efficiency.
Duplicate claims are one of the most overlooked causes of denials and compliance risks in healthcare billing.
AI-powered claim scrubbers can intelligently identify duplicate billing attempts across encounter dates, procedure combinations, claim types, insurance submissions, and provider records. This reduces compliance exposure while preventing unnecessary claim rejections and payment delays.
| Comparison Area | Traditional Claim Scrubber | AI Claim Scrubber Management Software |
| Validation Approach | Performs rule-based validation sequentially, checking one condition at a time | Performs real-time multi-layer AI validation across payer rules, coding edits, compliance checks, and authorization requirements simultaneously |
| Processing Speed | Slower validation process that may require manual review cycles | Validates claims in under a few seconds using automated AI-powered workflows |
| Documentation Review | Depends heavily on manual staff review of clinical documentation | Uses NLP-powered analysis to automatically review physician notes, treatment records, and clinical summaries |
| Coding Accuracy | Detects only predefined coding errors based on static logic | Continuously learns coding patterns and identifies hidden coding inconsistencies proactively |
| Payer Rule Management | Requires manual updates whenever payer policies change | Self-learning AI engine adapts automatically based on denial history and payer behavior |
| Denial Prevention Strategy | Reactive approach that catches errors after claim generation | Predictive approach that identifies denial probability before submission |
| Error Resolution | Flags claim issues without providing detailed correction guidance | Suggests correct codes, modifiers, documentation updates, and payer-specific fixes automatically |
| Claim Prioritization | All claims follow the same workflow regardless of risk level | AI assigns denial risk scores and prioritizes high-risk claims for human review |
| Duplicate Claim Detection | Limited ability to detect duplicate claims across systems | Intelligently identifies duplicate billing patterns across encounter dates, providers, procedures, and insurance submissions |
| Learning Capability | Static system with no continuous improvement mechanism | Continuously improves through machine learning and historical claim analysis |
| Workflow Automation | Supports partial automation with significant manual intervention | Provides intelligent end-to-end workflow automation with minimal human dependency |
| Analytics and Reporting | Offers basic reports with limited operational insights | Provides predictive analytics, denial trends, payer intelligence, and revenue cycle forecasting |
| Compliance Monitoring | Requires manual monitoring for HIPAA and payer compliance updates | Automatically validates claims against evolving compliance rules and payer regulations |
| EHR and Billing Integration | Often struggles with disconnected healthcare systems | Supports seamless integration with EHRs, EMRs, billing systems, and FHIR/HL7 standards |
| Operational Efficiency | High administrative workload and slower claim processing | Reduces manual work, accelerates reimbursements, and improves operational productivity |
| Scalability | Difficult to scale efficiently for large healthcare organizations | Easily scalable for multi-hospital networks and enterprise healthcare systems |
| First Pass Claim Acceptance Rate | Lower acceptance rates due to delayed error detection | Significantly improves first pass claim acceptance through predictive AI validation |
| Revenue Cycle Impact | Higher denial rates and increased revenue leakage | Optimizes reimbursements, reduces denials, and improves overall revenue cycle performance |
The real difference between traditional and AI-powered claim scrubbers is not simply automation. It is intelligence, adaptability, predictive analysis, and the ability to continuously optimize reimbursement outcomes in real time.
Healthcare organizations investing in AI claim scrubber management software development gain a significant competitive advantage by reducing denials, accelerating reimbursements, and building future-ready revenue cycle operations.

Healthcare organizations investing in AI medical claim scrubber software development must focus on building a platform that not only detects billing errors but also improves operational efficiency, compliance management, and reimbursement accuracy. The right feature architecture directly impacts clean claim rates, denial reduction, and revenue cycle performance.
If you are planning custom AI claim scrubber management software development for your hospital billing department and want to improve your clean claim rate above 95%, the following core modules and features should be included during the development process.
| Core Feature | Explanation |
| AI-Powered Claim Validation Engine | This feature automatically validates claims against payer-specific billing rules, coding regulations, authorization requirements, and compliance standards in real time, helping healthcare organizations reduce preventable denials and improve claim accuracy before submission. |
| Predictive Denial Analytics | Predictive analytics uses machine learning models to analyze historical denials, payer behavior, and coding trends to identify high-risk claims before submission, allowing billing teams to resolve issues proactively instead of reactively. |
| ICD-10 and CPT Code Validation | The software should automatically validate diagnosis and procedure codes to detect mismatches, invalid combinations, missing modifiers, and outdated coding structures that frequently cause healthcare claim denials and reimbursement delays. |
| NLP-Based Clinical Documentation Analysis | Natural Language Processing helps the system analyze physician notes, treatment summaries, and clinical records to identify missing medical necessity details and documentation gaps that could trigger claim rejection by insurance providers. |
| Real-Time Eligibility Verification | This module verifies patient insurance coverage, policy status, co-pay details, authorization requirements, and payer eligibility conditions instantly, helping billing departments avoid claim denials caused by outdated or inaccurate insurance information. |
| Automated Workflow Management | Automated workflow routing ensures that claims with validation issues are automatically assigned to coders, billers, or compliance teams based on severity, reducing manual coordination and accelerating claim resolution processes significantly. |
| Payer-Specific Rule Engine | The software should support payer-specific reimbursement logic and continuously update validation workflows according to changing insurance policies, helping healthcare organizations maintain higher clean claim rates across multiple insurance providers. |
| AI-Based Auto-Correction Suggestions | Instead of simply identifying claim issues, the system should recommend proper modifiers, corrected diagnosis codes, missing documentation updates, and payer-specific adjustments that billing staff can apply instantly with minimal effort. |
| Duplicate Claim Detection | AI-powered duplicate detection identifies repeated submissions across claim types, encounter dates, procedure combinations, and provider records, helping healthcare organizations reduce compliance risks and unnecessary reimbursement delays effectively. |
| Compliance Management System | A built-in compliance engine helps healthcare organizations maintain alignment with HIPAA regulations, CMS guidelines, NCCI edits, and payer-specific compliance standards while minimizing legal and operational risks during claim processing. |
| EHR and EMR Integration | The platform should integrate seamlessly with Electronic Health Records and Electronic Medical Records systems to ensure real-time data synchronization, reduce duplicate entries, and improve overall billing accuracy across departments. |
| Revenue Cycle Analytics Dashboard | Advanced dashboards provide insights into denial trends, clean claim percentages, payer performance, reimbursement delays, coding accuracy, and revenue leakage patterns, enabling healthcare leaders to make data-driven operational decisions confidently. |
| Role-Based Access Control | Role-based access management allows administrators to define permissions for billing staff, coders, compliance officers, and finance teams, ensuring secure claim processing workflows and protecting sensitive patient healthcare information effectively. |
| Multi-Payer Claims Processing | The software should support claims management across multiple insurance providers simultaneously while adapting validation logic according to payer-specific requirements, reimbursement structures, and adjudication workflows for improved operational scalability. |
| Real-Time Notification and Alert System | Intelligent alerts notify billing teams about missing authorizations, documentation gaps, coding inconsistencies, claim risks, or payer policy conflicts immediately, allowing faster issue resolution and minimizing reimbursement cycle delays significantly. |
So, these are the most essential modules and capabilities healthcare organizations should prioritize during custom AI claim scrubber management software development to achieve cleaner claims, faster reimbursements, and denial rates below industry averages.
As healthcare reimbursement systems become increasingly complex, healthcare organizations must move beyond basic automation and focus on intelligent, predictive, and scalable AI-driven capabilities. Advanced functionality plays a major role in helping hospitals create AI claim scrubber software that detects coding errors before submission and improves reimbursement efficiency continuously.
Organizations exploring how to build payer-specific claim scrubber rule engine using AI should consider implementing the following advanced features to future-proof their revenue cycle management systems.
| Advanced Feature | Explanation |
| Self-Learning AI Rule Engine | A self-learning AI engine continuously adapts validation logic by analyzing historical denials, payer adjudication trends, coding updates, and reimbursement outcomes, making the claim scrubber smarter and more accurate over time. |
| Predictive Reimbursement Forecasting | This feature uses AI models to estimate reimbursement probability, expected payment timelines, and financial outcomes before claim submission, helping healthcare organizations prioritize high-value claims and optimize revenue cycle performance strategically. |
| AI-Powered Fraud Detection | Advanced fraud detection algorithms analyze unusual billing behaviors, duplicate claim patterns, suspicious coding activities, and abnormal reimbursement trends to identify potential compliance violations and fraudulent healthcare claim submissions automatically. |
| Voice-Assisted Clinical Validation | Voice-enabled AI assistants can help physicians and billing teams validate coding accuracy, missing documentation, and medical necessity requirements through conversational workflows, improving efficiency and reducing administrative burden during claim preparation. |
| Behavioral Payer Intelligence System | This feature studies payer-specific adjudication patterns, approval behaviors, denial triggers, and reimbursement tendencies to optimize validation logic and improve claim acceptance rates across different insurance providers continuously. |
| Explainable AI Decision Framework | Explainable AI provides transparent reasoning behind claim validation decisions, denial predictions, and auto-correction recommendations, helping billing teams and compliance officers understand how the AI system reaches operational conclusions accurately. |
| Autonomous Denial Management | Autonomous denial management systems automatically analyze denied claims, identify root causes, generate correction recommendations, and initiate resubmission workflows without requiring significant manual intervention from revenue cycle management teams. |
| Real-Time Regulatory Update Engine | This module continuously monitors updates related to HIPAA, CMS, NCCI edits, payer policies, ICD coding standards, and healthcare compliance regulations to ensure claims validation workflows always remain fully updated automatically. |
| AI-Powered Claim Prioritization | Advanced AI algorithms categorize claims based on denial risk, reimbursement value, urgency, and payer behavior, enabling healthcare organizations to focus human review efforts where they deliver the highest financial impact. |
| Multi-Hospital Scalability Architecture | Enterprise-grade architecture allows healthcare organizations to manage claims workflows across multiple hospitals, clinics, and healthcare facilities while maintaining centralized analytics, payer intelligence, compliance monitoring, and operational consistency efficiently. |
So, these advanced AI-driven capabilities are becoming critical for healthcare organizations aiming to build future-ready claim scrubber platforms that maximize reimbursement accuracy, automate revenue cycle workflows, and maintain consistently high clean claim rates.
Healthcare organizations cannot improve clean claim rates simply by adding another billing tool into existing workflows. Building an intelligent claim scrubbing platform requires a structured development strategy that combines healthcare billing expertise, machine learning, workflow automation, payer intelligence, and strong operational usability.
Many healthcare leaders, insurance providers, and startup founders ask:
“We are looking for an experienced AI healthcare software development company that can help us create a custom AI claim scrubber system with predictive denial prevention, real-time claim validation, workflow automation, and payer-specific billing intelligence. What are the major stages involved in building this type of platform successfully?”
The answer lies in following a carefully planned development process that ensures scalability, prediction accuracy, compliance readiness, workflow adoption, and long-term operational value across healthcare revenue cycle management systems.

The first step in AI claim scrubber management software development is understanding how current billing and scrubbing workflows operate inside the organization. Before building any technology, the development team must analyze existing operational inefficiencies, denial patterns, payer-specific workflows, and coding validation gaps that are impacting reimbursement performance.
This stage involves auditing current scrubbing tools, identifying missing rule library coverage, reviewing specialty-specific billing behaviors, and understanding how claims move through the revenue cycle process. Teams also define measurable success metrics such as target clean claim rates, denial reduction percentages, and rework reduction goals.
A strong discovery phase ensures the software is built around real operational pain points rather than generic assumptions about healthcare billing workflows.
AI systems depend heavily on historical claims data to learn denial patterns and validation logic accurately. During this stage, healthcare organizations collect and organize 12 to 24 months of claims history including coding patterns, denial reasons, payer responses, reimbursement outcomes, authorization issues, and resubmission records.
The development team evaluates data quality, removes inconsistencies, standardizes formats, and prepares a clean training dataset for machine learning models. Poor or fragmented data during this phase can reduce AI prediction accuracy later in the project.
This step is especially important for organizations planning to develop automated claim data scrubbing engine capabilities that can continuously learn from operational billing data and improve validation performance over time.
PoC development helps healthcare organizations validate whether the AI validation engine can actually perform accurately using real claims data before committing to full-scale product development. This stage focuses on building a lightweight version of the core AI model and testing it against a sample claims dataset.
The objective is to measure:
This phase also helps identify technical limitations early while development costs remain manageable. A successful proof of concept gives operational stakeholders confidence that the system can improve clean claim rates and reduce manual billing workload effectively before expanding into enterprise-scale implementation.
Once the proof of concept is validated, the development team begins building the complete AI architecture for the platform. This stage includes training machine learning models for denial prediction, coding validation, risk scoring, and payer-specific billing intelligence using historical adjudication data.
Natural Language Processing models are also developed to analyze clinical notes, billing documentation, denial explanations, and payer communication automatically. At the same time, engineers build self-learning payer rule engines that continuously adapt to reimbursement policy changes and historical payer behavior patterns.
Organizations planning to develop AI-powered claim scrubbing software require this stage to ensure the system becomes smarter over time instead of functioning like a static rule-based billing tool.
Even highly advanced AI billing systems fail when billing teams struggle to use them comfortably in daily workflows. This is why UI/UX design becomes one of the most important stages in the development process of AI claim scrubber management system platforms.
The design team creates intuitive dashboards, real-time error queues, smart worklists, risk score indicators, one-click correction workflows, and operational reporting screens that align naturally with billing team behavior. The focus is reducing cognitive load while improving workflow speed and operational clarity.
Partnering with an experienced UI/UX design company ensures the product feels operationally practical, improves user adoption rates, and supports billing productivity from the very first day of deployment.
MVP development focuses on building the most valuable and operationally essential features first before investing in advanced capabilities. Instead of attempting to build a highly complex platform immediately, organizations launch a minimum viable product that solves the biggest claim validation and clean claim rate problems initially.
The MVP usually includes:
Top AI development companies often recommend this approach because it allows healthcare organizations to validate ROI, collect operational feedback, and optimize workflows before expanding into full-fledge development of enterprise-level AI automation capabilities.
Also Read: Top 10 AI MVP Development Companies in USA
Healthcare billing systems process sensitive patient and reimbursement data, making compliance and cybersecurity critical throughout the development lifecycle. During this phase, engineers implement HIPAA-compliant security architecture to protect claims information and operational workflows.
The system includes:
Security frameworks are implemented before live claims data enters the environment. Organizations working with an AI claim scrubber management software development company should always prioritize compliance architecture early rather than treating it as a secondary feature later in development.
Before deployment, the software must go through extensive testing across functionality, performance, operational workflows, and AI prediction accuracy. This phase determines whether the platform is stable and reliable enough for real healthcare billing operations.
The QA process includes:
The AI engine is tested against held-out claims datasets to confirm it improves clean claim rates, reduces coding errors, and minimizes claim rework effectively. Organizations planning to develop smart claim scrubber workflow automation software should never skip this phase because operational reliability directly impacts reimbursement performance and billing efficiency.
These above development stages help healthcare organizations build scalable, intelligent, secure, and operationally effective AI claim scrubbing platforms that improve clean claim rates, reduce billing rework, and optimize long-term revenue cycle performance.
The cost of AI claim scrubber management software development depends on several factors, including platform complexity, AI capabilities, payer rule customization, healthcare compliance requirements, integrations, and workflow automation needs. A basic MVP for small clinics costs significantly less than an enterprise-grade AI-powered platform designed for multi-hospital networks.
On average, the cost to build AI claim scrubber management software ranges between $40,000 to $350,000+ depending on features, scalability, security architecture, and AI model sophistication.
| Software Type | Estimated Development Cost | Best Suitable For | Included Capabilities |
| Basic AI Claim Scrubber MVP | $40,000 – $70,000 | Small clinics and healthcare startups | Basic claim validation, ICD/CPT code checking, eligibility verification, simple dashboards, and limited workflow automation |
| Standard AI Claim Scrubber Platform | $70,000 – $120,000 | Mid-sized hospitals and billing companies | AI-powered validation, payer-specific rules, denial prediction, EHR integration, workflow automation, and reporting dashboards |
| Advanced AI Claim Scrubber Software | $120,000 – $200,000 | Large hospitals and healthcare enterprises | NLP documentation analysis, predictive denial analytics, AI auto-correction, compliance management, and advanced analytics |
| Enterprise AI Claim Scrubber Management System | $200,000 – $350,000+ | Multi-hospital networks and enterprise healthcare providers | Self-learning AI engine, multi-payer intelligence, fraud detection, autonomous denial management, cloud scalability, and enterprise-grade security |
| Custom AI-Powered Revenue Cycle Ecosystem | $350,000+ | Nationwide healthcare systems and insurance organizations | Fully customized AI workflows, advanced interoperability, predictive reimbursement forecasting, real-time compliance monitoring, and multi-location management |
| Cost Factor | Impact on Development Cost |
| AI and Machine Learning Complexity | Advanced predictive analytics and self-learning AI models increase development effort and infrastructure requirements |
| EHR and EMR Integrations | Integrating with multiple healthcare systems using HL7 and FHIR standards increases implementation complexity |
| Payer-Specific Rule Engine | Custom payer validation workflows require continuous rule management and intelligent automation architecture |
| Compliance and Security Requirements | HIPAA compliance, encryption, audit logging, and healthcare cybersecurity frameworks significantly influence development cost |
| Workflow Automation Features | Intelligent routing, automated approvals, and denial management modules require advanced backend engineering |
| Analytics and Reporting Dashboards | Real-time analytics, predictive insights, and revenue cycle visualization tools increase frontend and backend development efforts |
| Cloud Infrastructure and Scalability | Enterprise-grade cloud deployment, high availability, and scalable healthcare architecture increase operational and infrastructure expenses |
| Third-Party API Integrations | Insurance verification APIs, coding databases, and healthcare interoperability systems add integration and maintenance costs |
| Development Team Expertise | Experienced healthcare AI developers, compliance engineers, and data scientists typically increase project investment but improve long-term product quality |
| Maintenance and AI Retraining | Ongoing AI model optimization, security updates, and payer rule updates contribute to long-term operational expenses |
| Maintenance Area | Estimated Monthly Cost |
| Cloud Hosting and Infrastructure | $1,000 – $8,000+ |
| AI Model Monitoring and Retraining | $2,000 – $10,000+ |
| Security Monitoring and Compliance Updates | $1,500 – $7,000+ |
| Technical Support and Bug Fixes | $2,000 – $6,000+ |
| API and Third-Party Service Costs | $500 – $5,000+ |
So, the final cost of custom AI claim scrubber management software development largely depends on how intelligent, scalable, compliant, and automated you want your healthcare claims platform to become.

Also Read: AI Software Development Cost
Building an intelligent healthcare claims platform requires a strong technology stack that supports AI automation, healthcare interoperability, compliance management, predictive analytics, and real-time claims validation. Healthcare organizations planning AI claim scrubber management software development must choose technologies that ensure scalability, security, high processing speed, and seamless integration with existing healthcare systems.
If you are planning to build NPI and patient eligibility validation software with AI, the following tools and technologies are considered essential for creating a secure, scalable, and future-ready AI-powered healthcare claims management platform.
| Technology Category | Tools and Technologies | Role in AI Claim Scrubber Management Software |
| Frontend Development Technologies | React.js, Angular, Vue.js | These frontend frameworks help build responsive dashboards, claims management portals, analytics interfaces, and real-time workflow monitoring systems for billing teams, coders, compliance officers, and healthcare administrators. |
| Backend Development Frameworks | Node.js, Python, Java, .NET | Backend technologies manage claims processing workflows, AI integrations, payer rule validation, business logic, API communication, and secure healthcare data handling across large-scale healthcare environments. |
| Artificial Intelligence and Machine Learning Frameworks | TensorFlow, PyTorch, Scikit-learn | AI and machine learning frameworks power predictive denial analytics, self-learning payer rule engines, coding validation, reimbursement forecasting, fraud detection, and intelligent claim automation functionalities. |
| Natural Language Processing Technologies | spaCy, BioBERT, OpenAI APIs, NLTK | NLP technologies analyze physician notes, clinical documentation, discharge summaries, and treatment records to identify medical necessity gaps, coding inconsistencies, and documentation errors before claim submission. |
| Database Management Systems | PostgreSQL, MongoDB, MySQL, Snowflake | Databases securely store patient records, billing data, payer rules, denial history, reimbursement analytics, audit logs, and healthcare workflow information required for AI-driven claims processing systems. |
| Cloud Infrastructure Platforms | AWS, Microsoft Azure, Google Cloud Platform | Cloud platforms provide scalable infrastructure for hosting AI claim scrubber software while supporting data encryption, disaster recovery, high availability, healthcare compliance, and enterprise-level scalability requirements. |
| Healthcare Interoperability Standards | HL7, FHIR, X12 EDI | These healthcare communication standards enable seamless integration between EHRs, EMRs, insurance systems, laboratory platforms, billing software, and payer networks for real-time healthcare data exchange. |
| Eligibility Verification and NPI Validation APIs | CMS NPI Registry API, Availity API, Change Healthcare APIs | These APIs help healthcare organizations build NPI and patient eligibility validation software with AI by verifying provider credentials, patient insurance coverage, payer eligibility status, and authorization requirements instantly. |
| Medical Coding and Billing Standards | ICD-10, CPT, HCPCS, NCCI Edits | Coding standards are essential for validating diagnosis codes, procedure combinations, modifier usage, and compliance requirements while reducing coding errors and preventing insurance claim denials effectively. |
| Workflow Automation Technologies | Camunda, Apache Airflow, UiPath | Workflow automation tools streamline claims routing, task assignments, approval cycles, denial management workflows, and operational coordination between billing teams, coders, and compliance departments automatically. |
| Real-Time Analytics and BI Tools | Power BI, Tableau, Looker | Analytics platforms provide dashboards for tracking clean claim rates, denial trends, payer performance, reimbursement cycles, coding accuracy, and operational efficiency across healthcare revenue cycle management systems. |
| API Development and Management Tools | REST APIs, GraphQL, Postman, Swagger | API technologies enable secure communication between healthcare platforms, payer systems, eligibility verification services, billing applications, and third-party healthcare software integrations efficiently. |
| Security and Compliance Technologies | OAuth 2.0, AES-256 Encryption, SIEM, MFA | Security frameworks protect sensitive healthcare data, maintain HIPAA compliance, enforce access controls, and prevent unauthorized access, cyberattacks, and healthcare data breaches across the platform infrastructure. |
| DevOps and Deployment Technologies | Docker, Kubernetes, Jenkins, GitHub Actions | DevOps tools automate software deployment, infrastructure management, continuous integration, scalability optimization, system monitoring, and operational maintenance for enterprise healthcare AI applications efficiently. |
| AI Model Monitoring and MLOps Tools | MLflow, Kubeflow, SageMaker | MLOps technologies monitor AI model performance, automate retraining processes, manage prediction accuracy, and ensure continuous optimization of denial prediction and claim validation algorithms over time. |
| Fraud Detection and Risk Analysis Tools | SAS Fraud Management, DataRobot, H2O.ai | Fraud analytics tools help identify suspicious billing activities, duplicate claims, abnormal reimbursement patterns, and compliance risks through advanced AI-driven behavioral analysis and anomaly detection systems. |
| Notification and Communication Services | Twilio, SendGrid, Firebase Notifications | Communication technologies deliver real-time alerts related to claim errors, eligibility issues, missing authorizations, denial risks, and workflow updates to healthcare billing teams instantly. |
| Audit Logging and Compliance Tracking Systems | Elastic Stack, Splunk, Datadog | Audit and monitoring tools track user activity, compliance events, claim modifications, system access logs, and workflow changes to support healthcare regulatory compliance and operational transparency. |
So, selecting the right technologies and healthcare AI infrastructure is one of the most critical steps in successful AI claim scrubber management software development because the platform’s performance, scalability, compliance readiness, and denial prevention capabilities depend heavily on the underlying technology stack.
Healthcare organizations investing in AI claim scrubber management software development must track the right KPIs to understand whether the platform is actually improving reimbursement accuracy, reducing denials, and optimizing revenue cycle workflows. Measuring performance through data-driven KPIs helps hospitals identify operational gaps and continuously improve claim processing efficiency.
For organizations planning custom AI medical claim scrubber software development, the following are the most important KPIs to measure long-term success and achieve clean claim rates above 95%.
Clean claim rate is one of the most critical KPIs for measuring the success of AI claim scrubber management software. It tracks the percentage of claims submitted without errors, missing documentation, coding issues, or payer conflicts.
A high clean claim rate indicates that the AI-powered validation engine is effectively identifying claim risks before submission. Healthcare organizations that develop smart claim scrubber workflow automation software typically aim to achieve clean claim rates above 95% to reduce rework and accelerate reimbursements.
This KPI measures how many claims are approved during the very first submission attempt without requiring corrections or resubmissions.
A strong first pass claim acceptance rate directly reflects how accurately the AI platform validates:
Organizations exploring how to create an AI claim scrubber tool that improves first pass claim acceptance rates should prioritize predictive AI validation and real-time claim analysis capabilities.
Claim denial rate measures the percentage of claims rejected by insurance payers.
One of the primary goals of AI medical claim scrubber software development is reducing denial rates through predictive intelligence, coding automation, and payer-specific validation workflows.
A decreasing denial rate usually indicates that the AI platform is successfully detecting:
before claims reach the payer.
Coding accuracy is a major KPI because coding errors remain one of the largest causes of healthcare claim denials.
This KPI measures how accurately diagnosis codes, procedure codes, modifiers, and billing combinations are applied during claim generation.
Healthcare organizations investing in custom AI claim scrubber management software development often use AI-powered coding validation and NLP-based documentation analysis to improve coding precision and reduce compliance risks significantly.
This KPI tracks how long it takes for healthcare providers to receive payments after claim submission.
AI-powered claim scrubbers improve reimbursement cycle time by:
A shorter reimbursement cycle improves cash flow and overall revenue cycle performance for hospitals and healthcare enterprises.
Denial prevention rate measures how effectively the software identifies and resolves claim risks before submission.
Unlike traditional scrubbers that react after errors occur, AI-powered systems proactively prevent denials using:
This KPI is especially important for healthcare organizations looking to build AI claim scrubber software that detects coding errors before submission.
Workflow automation efficiency measures how much of the claims management process is automated through AI.
This includes automation of:
Healthcare organizations developing AI claim scrubbing platform for insurance workflows often use this KPI to evaluate operational efficiency improvements and reductions in administrative workload.
ROI is the ultimate KPI that determines whether the investment in AI claim scrubber management software development is financially successful.
This KPI evaluates:
A strong ROI indicates that the AI-powered platform is delivering measurable business value while improving overall healthcare revenue cycle management performance.
So, these major KPIs help healthcare organizations measure whether their AI claim scrubber management software is truly improving clean claim rates, reducing denials, accelerating reimbursements, and optimizing end-to-end revenue cycle operations.
AI claim scrubber management software development offers enormous benefits for healthcare organizations, but building an intelligent, scalable, and compliant healthcare claims platform comes with several technical and operational challenges. Since healthcare billing ecosystems involve sensitive patient data, evolving payer regulations, and complex reimbursement workflows, even small development gaps can impact clean claim rates and operational efficiency significantly.
Healthcare organizations planning custom AI claim scrubber management software development must understand these challenges early to build a secure, accurate, and future-ready platform that consistently improves first pass claim acceptance rates.
Below are the major challenges healthcare enterprises face while developing AI claim scrubbing platform for insurance and hospital revenue cycle management systems, along with practical ways to overcome them.

Healthcare claims systems must comply with strict regulations such as:
The biggest challenge is that these regulations continuously evolve, making it difficult to maintain real-time compliance across claims workflows.
How to Overcome It: Development teams should implement automated compliance monitoring systems and real-time regulatory update engines. Using AI-powered validation workflows that continuously adapt to payer and regulatory changes helps healthcare organizations reduce compliance risks significantly.
AI systems are only as effective as the quality of data they receive.
In healthcare environments, patient records, coding data, and billing information often contain:
Poor-quality data reduces AI prediction accuracy and increases denial risks.
How to Overcome It: Organizations should build strong data cleansing, normalization, and validation pipelines before training AI models. Integrating standardized healthcare interoperability frameworks like HL7 and FHIR also improves data consistency across systems.
Healthcare organizations typically use multiple disconnected systems for billing, patient records, insurance verification, and clinical documentation.
Integrating AI claim scrubber management software with various EHRs, EMRs, and payer systems becomes technically challenging due to incompatible data structures and workflow dependencies.
How to Overcome It:
Development teams should adopt API-first architecture and support healthcare interoperability standards such as:
This ensures smoother integration between healthcare platforms and reduces operational silos.
One of the biggest challenges in AI medical claim scrubber software development is training machine learning models that can accurately predict denials, validate claims, and identify coding inconsistencies.
Healthcare reimbursement systems are highly dynamic, and payer behavior changes frequently.
How to Overcome It:
Organizations should continuously retrain AI models using:
Implementing MLOps frameworks helps maintain model accuracy and long-term AI performance.
Every insurance payer follows different reimbursement rules, authorization requirements, coding policies, and adjudication workflows.
Building a static validation engine cannot handle this level of complexity effectively.
How to Overcome It: Healthcare organizations should focus on how to build payer-specific claim scrubber rule engine using AI that continuously learns from payer behaviors and dynamically updates validation logic automatically.
Self-learning AI engines significantly improve claim validation accuracy across multiple insurance providers.
AI claim scrubber systems must validate large volumes of healthcare claims in real time without slowing down billing operations.
Poor system performance can create workflow bottlenecks and reimbursement delays.
How to Overcome It: Using scalable cloud infrastructure, distributed processing architecture, and optimized AI inference pipelines helps ensure high-speed claim validation even during peak operational loads.
Healthcare claims systems process highly sensitive patient and financial information, making cybersecurity a major challenge.
Healthcare organizations face increasing risks related to:
How to Overcome It:
Development teams should implement:
Strong cybersecurity architecture is essential for secure AI claim scrubber management software development.
Many billing teams and healthcare administrators hesitate to trust AI-driven automation because they fear losing control over claims processing workflows.
Lack of staff adoption can reduce the effectiveness of even the most advanced AI systems.
How to Overcome It:
Healthcare organizations should provide:
This helps employees understand how AI improves efficiency instead of replacing operational expertise.
As hospitals grow, AI claim scrubber systems must support increasing claim volumes, multiple departments, and multi-location healthcare operations.
Many platforms fail because they are not designed for enterprise scalability.
How to Overcome It: Organizations should use cloud-native architecture, microservices infrastructure, and scalable database systems that support multi-hospital deployment environments efficiently.
AI models can lose accuracy over time if they are not continuously updated according to changing payer rules, coding standards, and denial trends.
This issue is commonly known as AI model drift.
How to Overcome It: Healthcare organizations should implement continuous AI monitoring, automated retraining pipelines, and real-time performance analytics to maintain high validation accuracy and denial prediction performance over time.
So, understanding these major development challenges early helps healthcare organizations build smarter, more scalable, and highly accurate AI claim scrubber management software that delivers long-term operational efficiency and consistently higher clean claim rates.
Healthcare organizations today need more than a basic billing automation platform. They require intelligent healthcare revenue cycle systems that can predict denials, automate claim validation, improve coding accuracy, and continuously adapt to changing payer requirements. This is exactly where PixelBrainy helps hospitals, healthcare networks, and insurance-focused organizations modernize their claims management infrastructure.
Many healthcare enterprises often ask:
“We are searching for an AI insurance software solutions provider that specializes in healthcare claim scrubbing and billing automation. Who develops AI claim scrubber management software for healthcare providers?”
PixelBrainy delivers specialized healthcare AI solutions designed specifically for complex medical billing ecosystems, payer workflows, and enterprise-scale revenue cycle operations.
As an experienced AI development company, PixelBrainy focuses on building scalable healthcare automation systems that improve operational efficiency, reduce denials, and accelerate reimbursements through intelligent AI-powered workflows.
Their expertise in custom AI claim scrubber management software development helps healthcare providers:
PixelBrainy combines advanced technologies such as:
to develop intelligent claim error detection software that proactively identifies claim risks before submission.
The company also helps healthcare enterprises develop AI-driven claim scrubbing software capable of:
Unlike generic healthcare software vendors, PixelBrainy follows a healthcare-first engineering approach that prioritizes:
PixelBrainy partnered with a mid-sized multi-specialty hospital group struggling with:
The hospital network was operating with a clean claim rate of approximately 82%, resulting in significant revenue leakage and administrative overhead.
PixelBrainy developed a custom AI-powered claim scrubber platform that included:
Within six months of deployment, the hospital achieved:
The AI platform continuously learned from payer adjudication patterns, helping the hospital optimize claim accuracy and revenue cycle performance over time.
PixelBrainy’s healthcare AI engineering expertise allows healthcare organizations to move beyond traditional rule-based billing systems and adopt intelligent, future-ready claim automation platforms that maximize reimbursement efficiency and operational scalability.
Ready to improve your clean claim rate above 95% and modernize your healthcare billing workflows with AI-powered automation? Talk to PixelBrainy about developing your custom AI claim scrubber software tailored to your hospital, healthcare network, or revenue cycle management operations.

AI is rapidly transforming how healthcare organizations manage claims validation, billing automation, denial prevention, and revenue cycle optimization. Traditional rule-based claim scrubbers are no longer capable of handling the growing complexity of payer requirements, coding regulations, compliance standards, and reimbursement workflows.
Modern AI claim scrubber management software helps hospitals and healthcare providers improve clean claim rates, reduce claim denials, automate coding validation, accelerate reimbursements, and streamline operational efficiency through predictive intelligence and workflow automation.
Organizations investing in AI-powered healthcare claims solutions gain a major competitive advantage by minimizing revenue leakage, reducing administrative burden, and improving first pass claim acceptance rates significantly.
As healthcare reimbursement systems continue evolving, intelligent AI-driven claim scrubber platforms will become essential infrastructure for future-ready healthcare operations focused on scalability, compliance, financial performance, and long-term revenue cycle success.
Schedule a call with PixelBrainy to discuss your custom AI claim scrubber software development requirements and transform your healthcare claims workflow with intelligent automation.
AI claim scrubber management software is an intelligent healthcare billing solution that automatically validates medical claims before submission to insurance payers. It uses machine learning, predictive analytics, NLP, and workflow automation to identify coding errors, missing documentation, eligibility issues, duplicate claims, and payer-specific compliance risks. The software continuously learns from historical denials and payer behavior to improve clean claim rates and reduce reimbursement delays.
A claim scrubber focuses on identifying and correcting claim errors before submission, while a claim denial management system handles rejected claims after denial occurs. AI-powered claim scrubbers work proactively to prevent denials using predictive validation, whereas denial management systems work reactively to resolve payer rejections and resubmit claims for reimbursement.
Most healthcare organizations still struggle with low clean claim rates because traditional claim scrubbers rely on static rule engines and outdated workflows. These systems cannot predict payer behavior, analyze clinical documentation intelligently, or adapt to changing reimbursement policies. AI-powered claim scrubber management software improves clean claim rates by using predictive analytics, real-time validation, and self-learning payer intelligence.
Building AI claim scrubber software requires a combination of healthcare interoperability, machine learning, workflow automation, and compliance-focused architecture. The development process typically includes payer rule engine creation, AI model training, EHR integration, coding validation systems, eligibility verification workflows, predictive denial analytics, and HIPAA-compliant cloud infrastructure implementation.
The average cost of custom AI claim scrubber management software development ranges from approximately $40,000 to $350,000+ depending on the platform complexity, AI capabilities, healthcare integrations, compliance requirements, and scalability needs. Enterprise-grade healthcare claim automation systems with predictive analytics and multi-payer intelligence generally require larger development investments.
The development timeline depends on software complexity, AI functionality, integrations, and workflow customization requirements. A basic AI claim scrubber MVP may take around 5 to 8 weeeks, while advanced enterprise healthcare claims platforms with predictive denial analytics, NLP processing, and multi-payer workflow automation can take 9 to 14 weeks or longer.
AI claim scrubber software designed for multi-payer environments should include payer-specific rule engines, predictive denial scoring, eligibility verification, ICD-10 and CPT validation, NLP-powered documentation analysis, duplicate claim detection, workflow automation, real-time compliance updates, denial analytics dashboards, and scalable interoperability support using FHIR and HL7 standards.
PixelBrainy develops custom AI claim scrubber management software for hospitals, healthcare providers, insurance organizations, and revenue cycle management companies. The company specializes in AI-powered healthcare billing automation, predictive denial prevention, intelligent coding validation, payer-specific workflow automation, and scalable healthcare revenue cycle solutions.
About The Author
Sagar Bhatnagar
Sagar Sahay Bhatnagar brings over a decade of IT industry experience to his role as Marketing Head at PixelBrainy. He's known for his knack in devising creative marketing strategies that boost brand visibility and market influence. Sagar's strategic thinking, coupled with his innovative vision and focus on results, sets him apart. His track record of successful campaigns proves his ability to utilize digital platforms effectively for impactful marketing efforts. With a genuine passion for both technology and marketing, Sagar continuously pushes PixelBrainy's marketing initiatives to greater success.


Transform your ideas into reality with us.
Working with the PixelBrainy team has been a highly positive experience. They understand the design requirements and create beautiful UX elements to meet the application needs. The dev team did an excellent job bringing my vision to life. We discussed usability and flow. Sagar worked with his team to design the database and begin coding. Working with Sagar was easy. He has the knowledge to create robust apps, including multi-language support, Google and Apple ID login options, Ad-enabled integrations, Stripe payment processing, and a Web Admin site for maintaining support data. I'm extremely satisfied with the services provided, the quality of the final product, and the professionalism of the entire process. I highly recommend them for Android and iOS Mobile Application Design and Development.

Great experience working with them. Had a lot of feedback and I found that unlike most contractors they were bugging me for updates instead of the other way around. They were extremely time conscience and great at communicating! All work was done extremely high quality and if not on time, early! They were always proactive when it comes to communication and the work is great/above par always. Very flexible and a great team to work with! Goes above and beyond to present us with multiple options and always provides quality. Amazing work per usual with Chitra. If you have UI/UX or branding design needs I recommend you go to them! Will likely work with them in the future as well, definitely recommended!

PixelBrainy is a joy to work with and is a great partner when thinking through branding, logo, and website layout. I appreciate that they spend time going into the "why" behind their decisions to help inform me and others about industry best practices and their expertise.

I hired them to design our software apps. Things I really like about them are excellent communication skills, they answer all project suggestions and collaborate right away, and their input on design and colors is amazing. This project was complex and needed patience and creativity. The team is amazing to do business with. I will be using them long-term. Glad to see there are some good people out there. I was afraid to try and outsource my project to someone but I am glad I met them! I really can't say enough. They went above and beyond on this project. I am very happy with everything they have done to make my business stand out from the competition.

It was great working with PixelBrainy and the team. They were very responsive and really owned the project. We'll definitely work with them again!

I recently worked with the PixelBrainy team on a project and I was blown away by their communication skills. They were prompt, clear, and articulate in all of our interactions. They listened and provided valuable feedback and suggestions to help make the project a success. They also kept me updated throughout the entire process, which made the experience stress-free and enjoyable.

PixelBrainy is very good at what it does. The team also presents themselves very professionally and takes care of their side of things very well. I could fully trust them taking up the design work in a timely and organised manner and their attention to detail saved us lots of effort and time. This particular project was quite intense and the team showed that they function very well under pressure. Very much looking forward to working with her again!

It's always an absolute pleasure working with them. They completed all of my requests quickly and followed every note I had for them to a T, which made our process go smoothly from start to finish. Everything was completed fast and following all of the guidelines. And I would recommend their services to anyone. If you need any design work done in the future, PixelBrainy should be your first call!

They took ownership of our requirements and designed and proposed multiple beautiful variants. The team is self-motivated, requires minimum supervision, committed to see-through designs with quality and delivering them on time. We would definitely love to work with PixelBrainy again when we have any requirements.

PixelBrainy was a big help with our SaaS application. We've been hard at work with a new UI/UX and they provided a lot of help with the designs. If you're looking for assistance with your website, software, or mobile application designs, PixelBrainy and the team is a great recommendation.

PixelBrainy designers are amazing. They are responsive, talented, and always willing to help craft the design until it matches your vision. I would recommend them and plan to continue them for my future projects and more!!!

They were awesome! Did a good job fast, and good communication. Will work with them again. Thank you

Creative, detail-oriented, and talented designers who take direction well and implement changes quickly and accurately. They consistently over-delivered for us.

PixelBrainy team is very talented and creative. Great designers and a pleasure to work with. PixelBrainy is an excellent communicator and I look forward to working with them again.

PixelBrainy has a very talented design team. Their work is excellent and they are very responsive. I enjoy working with them and hope to continue on all of our future projects.
