Are you struggling with slow claim approvals, rising operational costs, and frequent errors in your healthcare claims process? If you are a healthcare provider, insurance company, or healthtech startup, this is a common challenge that directly impacts revenue and efficiency.
AI Medical Claims Processing Automation Software is a technology that uses artificial intelligence to automatically review, validate, and process healthcare insurance claims with minimal human intervention. It leverages machine learning, natural language processing (NLP), and OCR to handle complex medical data and streamline claim workflows.
The need for AI Medical Claims Processing Automation Software Development is growing rapidly as healthcare systems deal with increasing claim volumes and administrative pressure. According to Precedence Research, the global claims processing software market size was valued at USD 47.63 billion in 2025 and is expected to grow from USD 51.7 billion in 2026 to USD 108.09 billion by 2035, at a CAGR of 8.54%. This growth highlights the rising demand for automation and AI-driven solutions in claims management.
If you are exploring how to build AI medical claims processing software, the process involves designing intelligent systems that can extract data from medical documents, validate claims against insurance policies, and detect fraud patterns in real time. This makes building an AI Medical Claims Processing Automation Software both a technical and strategic investment.
Is AI medical claims automation profitable for healthcare businesses? Yes. By reducing manual intervention, minimizing errors, and accelerating claim approvals, AI significantly improves operational efficiency and return on investment.
The development of AI Medical Claims Processing Automation Software enables organizations to automate end-to-end claims workflows while improving accuracy, scalability, and compliance.
In this blog, you will learn about the architecture, tech stack, use cases, cost, and step-by-step approach to building an AI Medical Claims Processing Automation Software, helping you make informed technical and business decisions.
AI Medical Claims Processing Automation Software is a system that uses artificial intelligence to automatically capture, analyze, validate, and process healthcare insurance claims with minimal human intervention. It combines machine learning, natural language processing (NLP), and OCR to handle structured and unstructured medical data, enabling faster and more accurate claim decisions.
This software is designed for healthcare providers, insurance companies, and healthtech platforms that need to process large volumes of claims efficiently while reducing errors, fraud, and operational costs.
Purpose: Collects claim data from multiple sources
Ensures all claim-related data enters the system in a usable format.
Purpose: Converts unstructured documents into structured data
Critical for digitizing paper-based claims.
Purpose: Understands medical language and context
Enables accurate interpretation of complex healthcare data.
Purpose: Automate decision-making and predictions
Improves accuracy over time through continuous learning.
Purpose: Applies insurance policies and compliance rules
Combines with AI models for hybrid decision-making.
Purpose: Identify suspicious or duplicate claims
Essential for insurance risk management.
Purpose: Streamlines end-to-end claim processing
Speeds up claim lifecycle significantly.
Purpose: Connects with external systems
Enables seamless data exchange across systems.
Purpose: Provides visibility and analytics
Helps stakeholders make data-driven decisions.
Overall, AI Medical Claims Processing Automation Software automates the entire claims lifecycle using OCR, NLP, and machine learning, enabling faster processing, higher accuracy, and reduced operational costs for healthcare and insurance organizations.
Also Read: AI Medical Diagnosis Chatbot Development: Features and Cost
Medical claims processing is becoming increasingly complex due to rising claim volumes, manual workflows, and frequent errors. AI is needed to automate these processes, improve accuracy, and enable faster, more efficient claim handling at scale.
Medical claims processing is still largely dependent on manual review, fragmented systems, and rule-based validation. As claim volumes grow, this approach struggles to keep up with speed, accuracy, and scalability requirements.
Healthcare providers and insurers commonly deal with:
These issues directly impact revenue cycles, patient satisfaction, and overall efficiency.
Traditional claims processing systems are built on fixed rules and manual workflows.
They:
As a result, they become inefficient and costly over time.
AI introduces intelligent automation into the claims process.
It can:
This reduces manual work while improving speed and accuracy.
After adopting AI in medical claims processing:
AI is needed in medical claims processing to overcome delays, errors, fraud risks, and scalability issues by introducing automation, real-time decision-making, and intelligent data processing.
AI Medical Claims Processing Automation Software is transforming how healthcare organizations handle insurance claims by automating complex workflows, improving accuracy, and reducing operational costs. The growing adoption of AI in medical claims processing is driven by the need for faster claim approvals, fraud prevention, and scalable healthcare operations.
From hospitals to insurance companies, businesses are actively investing in AI Medical Claims Processing Automation Software Development to streamline claims workflows and enhance decision-making. Below are the most impactful use cases of AI healthcare claims automation systems.
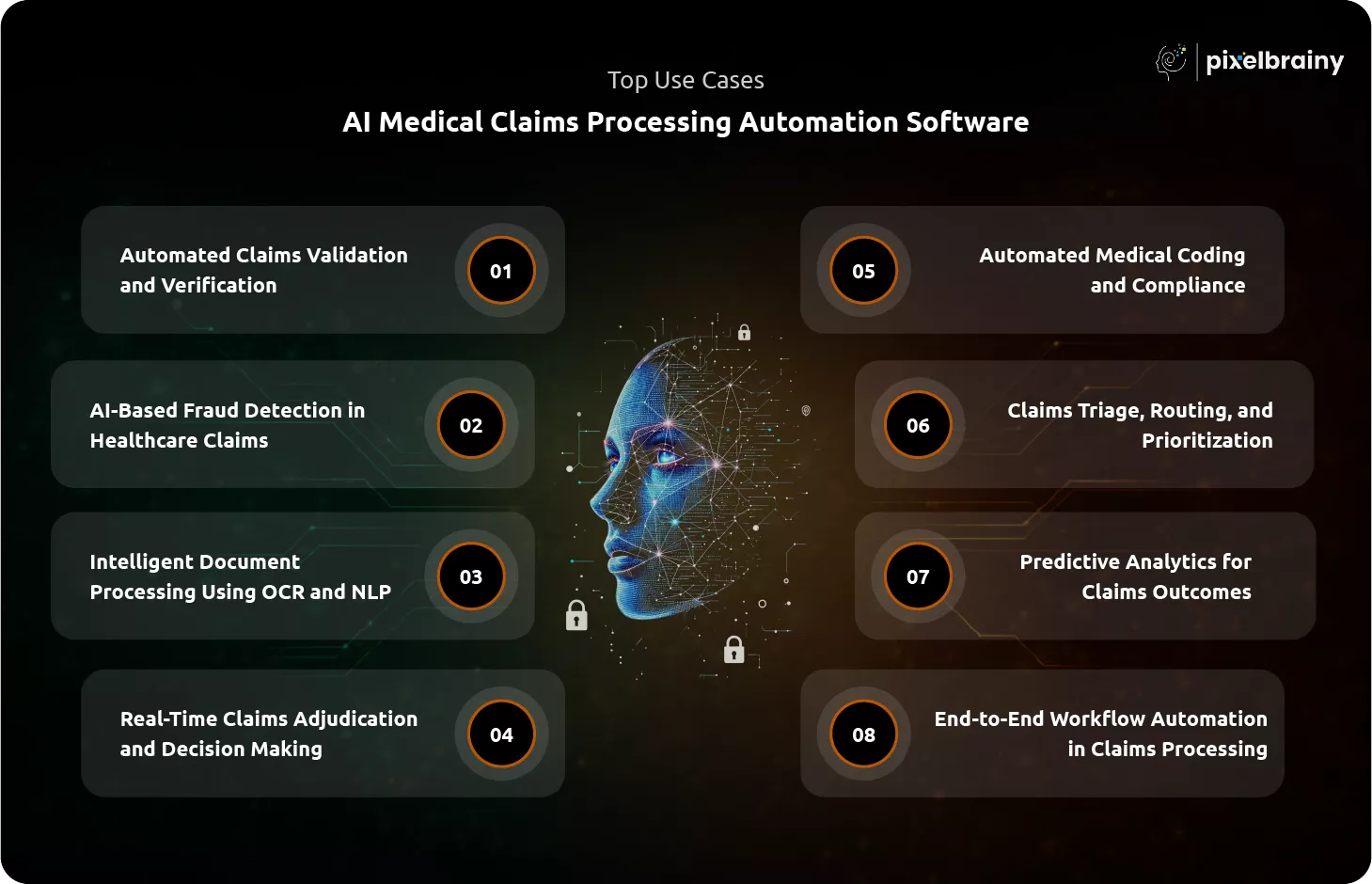
One of the most important use cases of AI medical claims processing software is automated validation of claims data.
AI systems automatically:
By using machine learning in insurance claims processing, organizations can significantly reduce claim rejections and improve approval rates.
This is a core function of any AI-based claims validation system.
Fraud detection is a major application of AI in healthcare insurance claims processing.
Using advanced algorithms, AI Medical Claims Processing Automation Software can:
This makes AI-powered claims processing software highly effective in minimizing financial risks and ensuring compliance.
A key benefit of AI healthcare claims automation is proactive fraud prevention.
Healthcare claims involve large volumes of unstructured documents such as prescriptions, invoices, and discharge summaries.
With AI medical claims automation systems, organizations can:
This capability is essential in building an AI Medical Claims Processing Automation Software, as it eliminates manual data entry and improves efficiency.
AI-powered claims adjudication enables real-time processing of insurance claims.
AI systems can:
This use case highlights how AI in medical claims processing improves speed and customer satisfaction.
Real-time adjudication is a major advantage of AI healthcare claims management systems.
Accurate coding is critical in healthcare billing.
AI Medical Claims Processing Automation Software helps by:
This is especially important in the development of AI Medical Claims Processing Automation Software, where accuracy directly impacts claim success rates.
AI enables intelligent handling of claims based on complexity and urgency.
Using AI-based claims processing systems, organizations can:
This improves operational efficiency in AI healthcare claims automation platforms.
Predictive analytics is a powerful feature of AI medical claims processing automation software.
AI models can:
This allows businesses to make data-driven decisions and optimize their healthcare claims automation strategy.
One of the biggest advantages of AI Medical Claims Processing Automation Software Development is complete workflow automation.
AI systems can automate:
This reduces manual effort and improves scalability in AI-powered healthcare claims processing systems.
These use cases demonstrate how AI Medical Claims Processing Automation Software streamlines claims workflows, enhances accuracy, and drives efficiency across healthcare and insurance operations.

Also Read: AI Medical Diagnosis App Development: Features & Cost
Developing AI Medical Claims Processing Automation Software enables healthcare providers and insurers to transform manual, error-prone workflows into intelligent, scalable, and efficient systems. As the demand for faster and more accurate claims handling grows, businesses are increasingly investing in AI medical claims processing software development to reduce costs, improve decision-making, and enhance operational performance.
By integrating technologies like machine learning, NLP, and automation, AI healthcare claims automation systems deliver measurable business value across the entire claims lifecycle. Below are the key business benefits of AI Medical Claims Processing Automation Software Development.
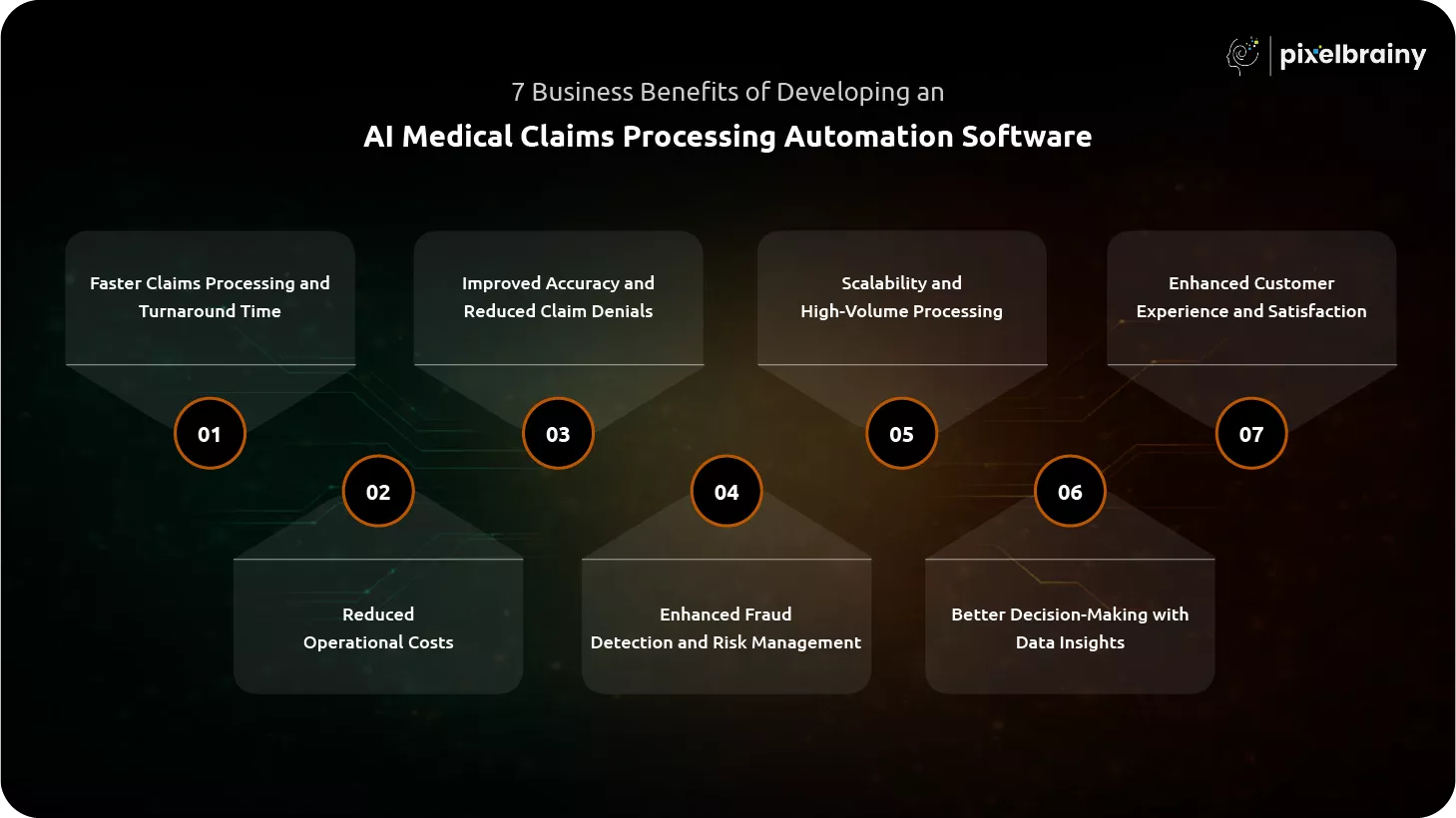
One of the biggest advantages of AI medical claims processing software is the ability to significantly reduce claim processing time. Traditional claims workflows involve multiple manual steps, which slow down approvals and reimbursements.
With AI in medical claims processing, tasks such as data extraction, validation, and adjudication are automated. This allows claims to be processed in real time or within hours instead of days. Faster turnaround improves operational efficiency and ensures quicker payments for healthcare providers.
As a result, organizations adopting AI healthcare claims automation can handle higher claim volumes without delays, leading to improved service delivery and better customer satisfaction.
AI Medical Claims Processing Automation Software Development helps businesses reduce administrative and operational costs. Manual claims processing requires a large workforce, increasing expenses related to staffing, training, and error correction.
By automating repetitive tasks, AI-based claims processing systems minimize the need for manual intervention. This reduces labor costs and eliminates inefficiencies caused by human errors.
Additionally, faster processing and fewer claim rejections lower the cost of rework. Over time, AI-powered healthcare claims processing software delivers strong cost savings and improves overall profitability for healthcare organizations and insurers.
Accuracy is critical in claims processing, and even small errors can lead to claim denials. AI medical claims automation systems improve accuracy by analyzing data consistently and applying validation rules without human bias.
Using machine learning in insurance claims processing, AI can detect missing information, incorrect coding, and inconsistencies before submission. This reduces the chances of rejection and ensures higher claim approval rates.
By improving data accuracy, AI Medical Claims Processing Automation Software helps organizations reduce rework, enhance compliance, and maintain better financial stability.
Fraud is a major challenge in healthcare insurance, costing businesses billions annually. AI in healthcare claims processing enables advanced fraud detection by analyzing patterns and identifying anomalies in real time.
Unlike traditional systems, AI-powered claims processing software can detect complex fraud scenarios such as duplicate claims, inflated billing, and suspicious activities. Machine learning models continuously improve by learning from new data.
This strengthens risk management and helps organizations prevent financial losses. Implementing AI healthcare claims automation systems ensures better compliance, transparency, and trust in the claims process.
As healthcare systems grow, the volume of claims increases significantly. AI Medical Claims Processing Automation Software allows businesses to scale operations without increasing workforce or infrastructure costs.
AI systems can process thousands of claims simultaneously, making them ideal for high-demand environments. This scalability is a key advantage of AI medical claims processing software development, especially for large hospitals and insurance companies.
By handling increased workloads efficiently, AI healthcare claims automation platforms support business growth and ensure consistent performance even during peak demand.
AI medical claims processing automation software provides valuable insights through data analysis and predictive modeling. Organizations can use these insights to improve decision-making and optimize operations.
AI systems analyze historical claims data to identify trends, predict outcomes, and highlight inefficiencies. This enables smarter strategies in pricing, policy management, and risk assessment.
With AI in medical claims processing, businesses gain real-time visibility into operations, allowing them to make informed decisions and improve overall performance.
Customer experience is a key factor in healthcare and insurance services. AI Medical Claims Processing Automation Software improves customer satisfaction by reducing delays and providing faster claim resolutions.
Patients and providers benefit from quicker approvals, transparent communication, and fewer errors. Automated updates and real-time tracking further enhance the experience.
By implementing AI healthcare claims automation systems, organizations can deliver seamless and reliable services, strengthening customer trust and long-term relationships.
These business benefits show that AI Medical Claims Processing Automation Software is a high-impact investment that drives efficiency, accuracy, scalability, and long-term profitability in healthcare claims management.
Also Read: How to Develop an AI Medicine Delivery App
AI Medical Claims Processing Automation Software Development focuses on building intelligent systems with essential features that automate, validate, and optimize the entire claims lifecycle. These features enable AI medical claims processing software to handle complex healthcare data, reduce manual effort, and improve operational efficiency.
To successfully build AI medical claims processing software, integrating the following core features is critical for performance, scalability, and compliance.
| Feature | Description |
| Data Ingestion System | This feature enables seamless collection of claims data from multiple sources such as EHR systems, billing platforms, and APIs. It ensures that both structured and unstructured data is captured efficiently. In AI healthcare claims automation systems, this acts as the foundation for accurate data processing. |
| OCR-Based Document Processing | OCR technology extracts text from scanned documents, invoices, and medical reports. It eliminates manual data entry and converts unstructured data into structured formats. This is a critical component in AI medical claims processing software development for handling paper-based claims. |
| NLP-Based Medical Text Understanding | NLP helps the system understand complex medical terminology from clinical notes and prescriptions. It identifies key entities like diagnosis, procedures, and treatments. This improves accuracy in AI medical claims automation systems. |
| Claims Validation Engine | This feature validates claims against insurance policies, eligibility criteria, and billing rules. It ensures that all required data is accurate and complete before submission. It plays a key role in AI-based claims validation systems. |
| Automated Adjudication System | This system automatically approves or rejects claims based on predefined rules and AI models. It reduces the need for manual review and speeds up claim processing. It is essential in AI-powered claims processing software. |
| Fraud Detection Module | The fraud detection module uses machine learning to identify suspicious patterns and anomalies in claims. It detects duplicate claims and unusual billing behaviors. This strengthens security in AI healthcare claims automation systems. |
| Medical Coding Automation | This feature automatically assigns ICD and CPT codes based on medical data. It reduces coding errors and ensures compliance with healthcare standards. It is a key part of AI medical billing and claims automation solutions. |
| Workflow Automation Engine | Workflow automation manages claim routing, approvals, and task assignments without manual intervention. It ensures smooth and efficient processing across the system. This enhances productivity in AI claims processing automation systems. |
| Real-Time Processing Capability | Real-time processing allows instant validation and decision-making for claims. It significantly reduces turnaround time and improves responsiveness. This feature is vital in modern AI medical claims processing software. |
| Integration APIs | Integration APIs connect the software with hospital systems, insurance platforms, and third-party services. They enable seamless data exchange across systems. This is essential in AI claims processing software development. |
| Dashboard and Analytics | This feature provides real-time insights into claim status, performance metrics, and trends. It helps stakeholders monitor operations and make informed decisions. It is widely used in AI healthcare analytics systems. |
| Compliance Management System | This system ensures adherence to healthcare regulations such as HIPAA and GDPR. It monitors processes and maintains compliance standards. It is critical in AI healthcare software development. |
| Data Security and Encryption | Data security features protect sensitive patient and claims information through encryption and secure storage. It ensures confidentiality and integrity of data. This is essential in AI medical claims processing automation software. |
| Error Detection and Alerts | This feature identifies missing or incorrect data in claims and generates alerts. It helps prevent claim rejection and improves accuracy. It is a valuable component in AI claims automation systems. |
| Reporting and Audit Trails | This feature maintains detailed logs of all claim activities and transactions. It supports audits, compliance checks, and transparency. It is important for governance in AI medical claims processing systems. |
These core features enable AI Medical Claims Processing Automation Software to deliver efficient, accurate, and scalable claims management across healthcare and insurance ecosystems.
To stay competitive, organizations must go beyond basic functionality and adopt advanced capabilities. Building an AI Medical Claims Processing Automation Software with advanced features enables smarter automation, predictive intelligence, and enhanced decision-making.
These advanced capabilities strengthen the performance of AI healthcare claims automation systems and improve long-term business outcomes.
| Feature | Description |
| Predictive Analytics for Claims Outcomes | This feature uses machine learning models to predict claim approvals, denials, and processing delays. It helps organizations take proactive actions to improve outcomes. It enhances decision-making in AI medical claims processing software. |
| AI-Based Risk Scoring | Risk scoring assigns a probability score to each claim based on historical data and patterns. It helps prioritize high-risk or complex claims for review. This is important in AI claims risk management systems. |
| Explainable AI (XAI) | Explainable AI provides transparency by showing how decisions are made. It helps users understand why a claim was approved or rejected. This builds trust in AI healthcare claims automation systems. |
| Real-Time Fraud Detection | This feature identifies fraudulent activities during the claim processing stage. It uses advanced algorithms to detect anomalies instantly. It strengthens security in AI healthcare fraud detection systems. |
| Voice and Conversational AI Integration | This feature enables voice-based claim input and chatbot support. It improves user interaction and accessibility. It is useful in AI healthcare automation platforms. |
| Blockchain Integration for Security | Blockchain ensures secure and tamper-proof storage of claims data. It improves transparency and data integrity. It is an advanced capability in AI medical claims processing software. |
| Automated Compliance Monitoring | This feature continuously tracks regulatory requirements and updates workflows accordingly. It ensures compliance without manual intervention. It is essential in AI healthcare compliance systems. |
| Intelligent Claims Routing | Intelligent routing directs claims based on complexity, urgency, and risk level. It optimizes workflow and resource allocation. It improves efficiency in AI claims processing automation systems. |
| Multi-Language Processing | This feature allows the system to process claims in multiple languages. It supports global healthcare operations and improves accessibility. It is useful in AI global healthcare claims platforms. |
| Generative AI for Claim Summarization | Generative AI creates concise summaries of claims and medical records. It helps decision-makers quickly understand complex data. It is an emerging feature in AI medical claims processing automation software. |
Advanced features enhance AI Medical Claims Processing Automation Software by enabling intelligent automation, predictive insights, and scalable healthcare claims processing systems.
The step-by-step development of AI medical claims automation system requires a structured approach that combines healthcare domain knowledge, AI technologies, and scalable software engineering. If you are wondering what is the process to build an AI Medical Claims Processing Automation Software, it involves careful planning, data preparation, model development, and system integration.
This section explains a practical roadmap for developing an AI Medical Claims Processing Automation Software that is efficient, compliant, and scalable.
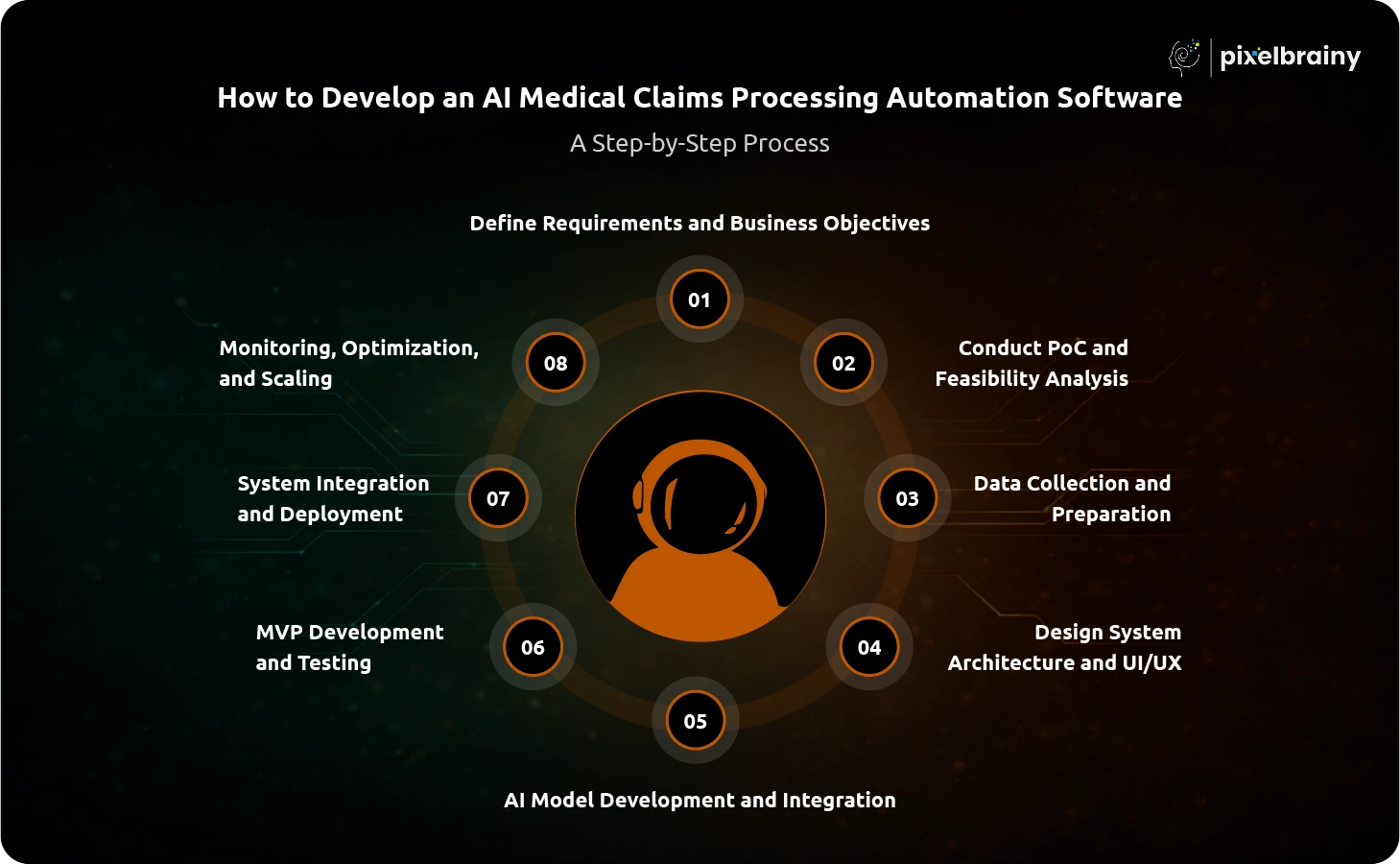
Aim: Establish a clear vision and use case for the solution
The first step in Medical Claims Processing Automation Software integrating AI is identifying business goals and system requirements. This includes understanding claim workflows, user needs, compliance requirements, and key pain points such as delays or fraud.
At this stage, organizations also evaluate Is AI medical claims automation profitable for healthcare businesses? by analyzing ROI, cost savings, and efficiency improvements. Clear requirements ensure the solution aligns with business outcomes.
Aim: Validate the technical and business feasibility of the solution
Before full-scale development, a PoC Development phase is essential to test core functionalities like OCR extraction, NLP processing, and AI validation models. This helps in identifying potential challenges and assessing model accuracy.
A successful proof of concept reduces risks and provides confidence in moving forward with full system development.
Aim: Build a high-quality dataset for training AI models
AI systems rely heavily on data. This step involves collecting medical records, billing data, and historical claims. The data is then cleaned, labeled, and structured for training purposes.
High-quality datasets are critical in developing an AI Medical Claims Processing Automation Software, as they directly impact model performance and accuracy.
Aim: Create a scalable and user-friendly system design
In this step, developers design the system architecture, including data pipelines, AI layers, and integration points. At the same time, collaboration with UI/UX design companies ensures the platform is intuitive and easy to use for healthcare staff.
A well-designed architecture improves scalability, while a strong interface enhances user adoption.
Aim: Build and integrate intelligent processing capabilities
This step involves developing machine learning models for claims validation, NLP models for medical text understanding, and OCR systems for document extraction. These components are integrated into the platform to enable automation.
Working with Top AI development companies can accelerate this phase and ensure robust model performance.
Aim: Build a functional version for real-world testing
An MVP allows businesses to launch a basic version of the system with essential features. Collaboration with MVP Development Companies helps accelerate this process and gather early feedback.
Testing ensures the system performs accurately under real conditions and identifies areas for improvement.
Aim: Deploy the solution and integrate with existing systems
The developed system is integrated with hospital management systems, insurance platforms, and third-party APIs. Deployment is typically done on cloud infrastructure for scalability.
This step ensures seamless data flow and enables real-time claim processing in production environments.
Aim: Continuously improve performance and scalability
After deployment, the system is monitored for performance, accuracy, and user feedback. AI models are retrained with new data to improve outcomes over time.
Continuous optimization ensures long-term success and scalability of the AI medical claims processing automation software.
The process to build AI Medical Claims Processing Automation Software includes requirement analysis, PoC validation, data preparation, architecture design, AI model development, MVP testing, system deployment, and continuous optimization to ensure scalable and efficient claims automation.
Also Read: AI Health Assessment App Development: A Complete Guide
The cost to build AI Medical Claims Processing Automation Software typically ranges from $30,000 to $300,000+, based on system complexity, AI capabilities, and business requirements. Organizations investing in AI medical claims processing software development must consider factors such as automation level, data processing needs, compliance, and integration with healthcare systems.
Understanding the cost of developing AI Medical Claims Processing Automation Software helps businesses plan budgets, estimate ROI, and choose the right development approach. Whether building a basic system or a fully advanced enterprise solution, the total investment depends on the scope and functionality of the software.
| Software Type | Description | Estimated Cost | Timeline |
| Basic AI Medical Claims Processing Automation Software | A basic system includes essential features such as data ingestion, OCR-based document processing, and simple claims validation. It is suitable for startups or small healthcare providers beginning with AI healthcare claims automation. The system focuses on automating repetitive tasks with limited AI capabilities. | $30,000 – $80,000 | 2 – 4 months |
| Medium AI Medical Claims Processing Automation Software | A mid-level solution includes advanced features such as NLP-based medical text processing, fraud detection, workflow automation, and system integrations. It is ideal for growing healthcare businesses adopting AI medical claims processing software for improved efficiency. The system offers better accuracy and scalability. | $80,000 – $180,000 | 4 – 8 months |
| Advanced AI Medical Claims Processing Automation Software | An advanced system includes enterprise-grade features such as predictive analytics, real-time claims adjudication, advanced fraud detection, and scalable cloud infrastructure. It is designed for large healthcare organizations and insurers using AI claims processing automation systems. The system delivers high performance, automation, and intelligence. | $180,000 – $300,000+ | 8 – 14+ months |
| Cost Factor | Description | Estimated Cost Impact |
| AI Model Development | Developing machine learning, NLP, and OCR models requires significant effort and expertise. The complexity of models directly impacts the cost of AI medical claims processing software development. Advanced models increase both time and budget. | $10,000 – $80,000+ |
| Data Collection and Preparation | High-quality data is essential for training AI models. This includes data cleaning, labeling, and structuring. Poor data quality can increase development time and cost. | $5,000 – $40,000 |
| Feature Complexity | The number and type of features, such as fraud detection, predictive analytics, and automation, significantly influence cost. More advanced features lead to higher development expenses. | $10,000 – $100,000+ |
| System Integration | Integration with hospital systems, insurance platforms, and third-party APIs adds complexity. The more integrations required, the higher the cost. | $5,000 – $50,000 |
| UI/UX Design | Designing a user-friendly interface improves usability and adoption. Complex dashboards and workflows increase design and development effort. | $3,000 – $20,000 |
| Cloud Infrastructure | Cloud services such as AWS, Azure, or Google Cloud are required for hosting and scalability. Costs depend on usage, storage, and computing power. | $5,000 – $30,000/year |
| Compliance and Security | Ensuring compliance with healthcare regulations like HIPAA and GDPR requires additional development and security measures. This increases overall cost. | $5,000 – $25,000 |
| Development Team Location | The cost varies depending on the region of the development team. Offshore teams are generally more cost-effective compared to US or European teams. | Varies (20%–60% difference) |
| Maintenance and Updates | Ongoing maintenance, system updates, and AI model retraining are necessary for long-term performance. These costs continue after deployment. | 15%–25% annually |
Investing in AI Medical Claims Processing Automation Software is a strategic decision that delivers long-term cost savings, operational efficiency, and scalable growth for healthcare and insurance organizations.

The development of AI Medical Claims Processing Automation Software requires a robust and scalable technology stack that supports data processing, AI model development, system integration, and secure deployment. Choosing the right tools is critical for building efficient and reliable AI medical claims processing software that can handle complex healthcare data and high claim volumes.
A well-defined technology stack for AI healthcare claims automation systems ensures better performance, faster development, and long-term scalability.
| Technology Area | Tools & Technologies | Description |
| Programming Languages | Python, JavaScript, Java | Python is widely used for AI medical claims processing software development due to its strong AI and ML libraries. JavaScript and Java are used for backend and frontend development. These languages ensure flexibility and scalability. |
| AI & Machine Learning Frameworks | TensorFlow, PyTorch, Scikit-learn | These frameworks are used to build machine learning models for claims validation, fraud detection, and predictive analytics. They enable intelligent automation in AI healthcare claims automation systems. |
| Natural Language Processing (NLP) | spaCy, Hugging Face Transformers, NLTK | NLP tools help understand medical text, clinical notes, and prescriptions. They are essential for extracting meaningful insights in AI medical claims processing systems. |
| OCR (Document Processing) | Tesseract OCR, AWS Textract, Google Vision AI | OCR tools extract text from scanned medical documents and invoices. They convert unstructured data into structured formats, which is crucial in AI claims processing software development. |
| Backend Development Frameworks | Django, Flask, FastAPI, Node.js | Backend frameworks handle server-side logic, APIs, and data processing. FastAPI and Django are popular for building scalable AI medical claims automation systems. |
| Frontend Development | React.js, Angular, Vue.js | Frontend technologies are used to build user interfaces and dashboards. They ensure a smooth user experience in AI healthcare claims processing software. |
| Database Systems | PostgreSQL, MongoDB, MySQL | Databases store structured and unstructured claims data securely. Choosing the right database improves performance in AI medical claims processing automation software. |
| Cloud Platforms | AWS, Microsoft Azure, Google Cloud Platform | Cloud platforms provide scalable infrastructure, storage, and computing power. They are essential for deploying AI claims processing automation systems. |
| API Integration Tools | REST APIs, GraphQL | APIs enable integration with hospital systems, insurance platforms, and third-party services. They ensure seamless data exchange in AI healthcare claims automation platforms. |
| Data Processing Tools | Apache Spark, Pandas, NumPy | These tools are used for large-scale data processing and analysis. They support efficient handling of healthcare data in AI medical claims systems. |
| Security & Compliance Tools | OAuth 2.0, SSL/TLS, HIPAA-compliant frameworks | These tools ensure data security, encryption, and compliance with healthcare regulations. They are critical in AI healthcare software development. |
| DevOps & Deployment Tools | Docker, Kubernetes, Jenkins | DevOps tools help in continuous integration, deployment, and scaling. They ensure smooth delivery of AI medical claims processing software. |
| Monitoring & Analytics Tools | Prometheus, Grafana, ELK Stack | These tools monitor system performance and provide real-time analytics. They help maintain efficiency in AI healthcare claims automation systems. |
Selecting the right tools and technology stack is essential for developing AI Medical Claims Processing Automation Software that delivers high performance, accuracy, and scalability in healthcare claims processing.
The business model of AI Medical Claims Processing Automation Software defines how companies generate revenue, deliver value, and scale their solutions in the healthcare and insurance industry. With the growing demand for AI medical claims processing software, organizations are adopting flexible and scalable monetization strategies to serve hospitals, insurers, and healthtech platforms.
Choosing the right business model is critical for maximizing ROI, ensuring long-term sustainability, and successfully commercializing AI healthcare claims automation systems.
The SaaS model is the most widely used approach in AI medical claims processing software development, where the software is hosted on the cloud and offered on a subscription basis. Customers access the platform via web or APIs without managing infrastructure.
Key Points:
In this model, businesses charge customers based on the number of claims processed using the AI claims processing automation system. It is ideal for organizations with fluctuating claim volumes.
Key Points:
The enterprise model involves selling a licensed version of AI medical claims processing automation software to large organizations. It is typically customized and deployed on-premise or private cloud.
Key Points:
In this model, companies offer custom AI medical claims processing software development services tailored to specific business requirements. Each solution is built from scratch based on client needs.
Key Points:
The freemium model offers basic features of AI healthcare claims automation software for free, while advanced features require a paid subscription. It is commonly used to attract new users.
Key Points:
This model provides AI capabilities such as OCR, NLP, and claims validation through APIs. Businesses integrate these APIs into their existing systems.
Key Points:
Selecting the right business model is essential for maximizing revenue, ensuring scalability, and successfully delivering AI Medical Claims Processing Automation Software to healthcare and insurance markets.
Also Read: AI Medication Assistant App Development: A Complete Guide
Despite the growing adoption of AI in medical claims processing, developing an AI Medical Claims Processing Automation Software is not without challenges. From handling complex healthcare data to ensuring regulatory compliance and system scalability, organizations must navigate multiple technical and operational hurdles.
Understanding these challenges early and implementing the right strategies is critical for building reliable, accurate, and scalable AI healthcare claims automation systems that deliver real business value.
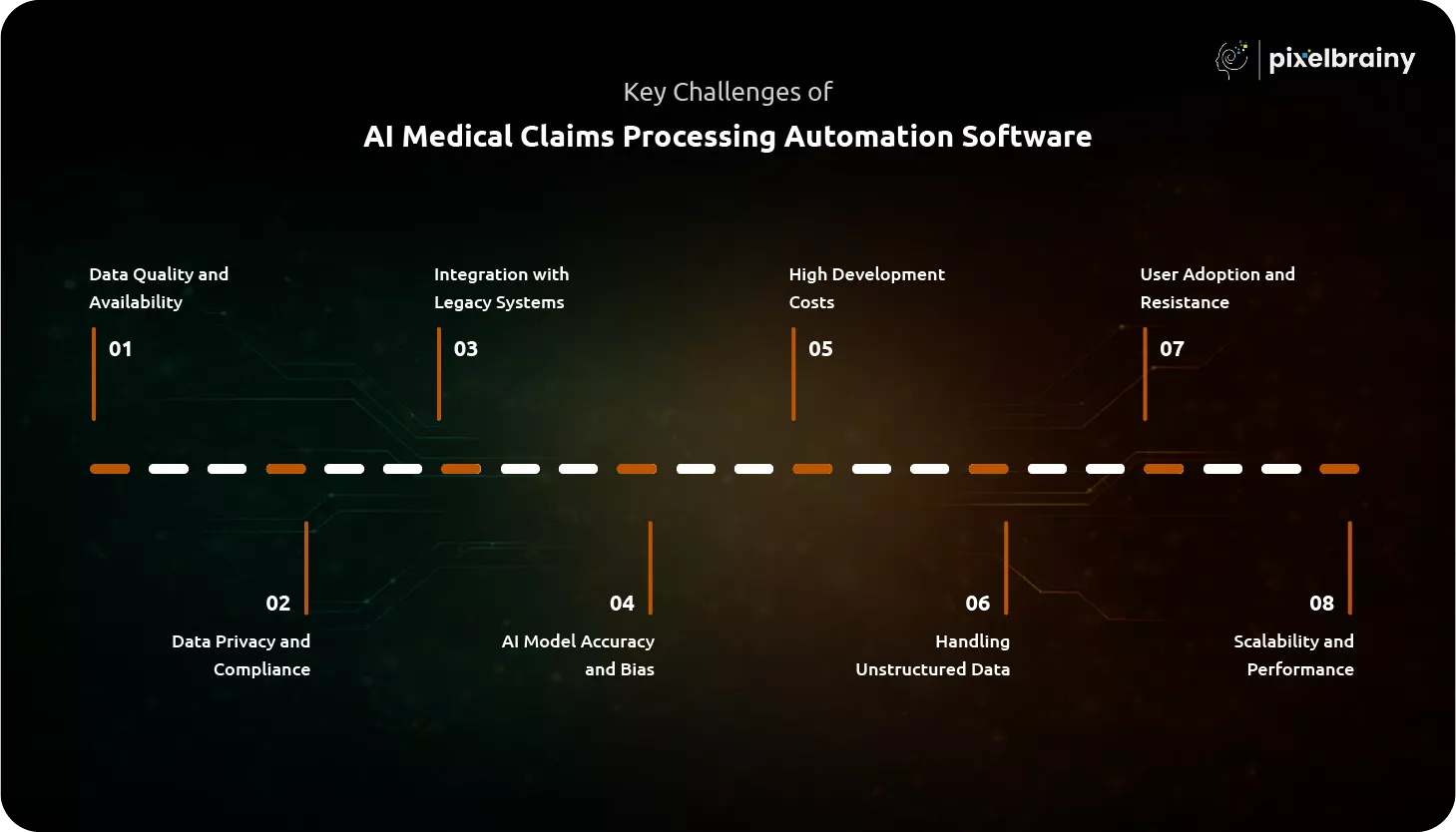
Challenge: Healthcare data is often incomplete, inconsistent, and unstructured, which directly impacts the performance of AI models. Poor data quality leads to inaccurate claim validation and higher rejection rates in AI medical claims processing software.
Solution: Organizations should implement strong data preprocessing pipelines, standardize data formats, and continuously update datasets. Using clean, labeled, and structured data ensures better model training and improves the accuracy of AI healthcare claims automation systems.
Challenge: Handling sensitive patient data requires strict compliance with regulations like HIPAA and GDPR. Ensuring data security while processing large volumes of claims is complex in AI medical claims processing automation software.
Solution: Businesses should implement encryption, access control mechanisms, and secure data storage. Regular audits and compliance monitoring help maintain regulatory standards and ensure safe handling of data in AI healthcare claims processing systems.
Challenge: Many healthcare organizations rely on outdated legacy systems that are not compatible with modern AI solutions. This creates challenges in integrating AI medical claims processing software with existing workflows.
Solution: Using APIs and middleware can help bridge the gap between legacy and modern systems. Adopting modular architecture and gradual system upgrades ensures smooth integration in AI healthcare claims automation platforms.
Challenge: AI models can produce inaccurate or biased results due to poor training data or limited datasets. This affects decision-making in AI medical claims processing automation systems.
Solution: Organizations should train models on diverse datasets and regularly validate performance. Implementing explainable AI and continuous retraining improves accuracy and reduces bias in AI claims processing software development.
Challenge: The cost of AI medical claims processing software development can be high due to AI model complexity, data preparation, and system integration requirements. This can limit adoption for smaller organizations.
Solution: Starting with an MVP, using pre-trained models, and leveraging cloud infrastructure can reduce costs. Prioritizing essential features helps optimize investment in AI healthcare claims automation systems.
Challenge: Medical claims include unstructured data such as handwritten notes, PDFs, and clinical reports. Processing this data accurately is difficult for traditional systems.
Solution: Using advanced OCR and NLP technologies helps extract and interpret unstructured data effectively. Continuous model improvement ensures better performance in AI medical claims processing software.
Challenge: Healthcare professionals may resist adopting AI systems due to lack of trust or familiarity. This slows down implementation of AI healthcare claims automation solutions.
Solution: Providing training, intuitive interfaces, and human-in-the-loop systems improves user confidence. Demonstrating real-world benefits encourages adoption of AI medical claims processing automation software.
Challenge: As claim volumes grow, systems must handle increased workloads without performance issues. Poor scalability affects efficiency in AI claims processing automation systems.
Solution: Using cloud-based infrastructure, microservices architecture, and performance monitoring ensures scalability. Continuous optimization supports long-term growth of AI medical claims processing software.
Overcoming these challenges is essential for building scalable, secure, and high-performing AI Medical Claims Processing Automation Software that delivers long-term value.
The success of building an AI Medical Claims Processing Automation Software depends heavily on selecting the right AI development company. A strong technology partner ensures that your solution is not only technically sound but also aligned with healthcare workflows, compliance requirements, and business goals.
PixelBrainy LLC helps organizations accelerate the development of AI Medical Claims Processing Automation Software by combining domain expertise with advanced AI technologies.
PixelBrainy follows a structured approach for Medical Claims Processing Automation Software Development Integrating AI, ensuring every stage is aligned with business outcomes.
The team specializes in developing intelligent healthcare systems using AI, ensuring high accuracy and performance in claims processing.
PixelBrainy builds systems designed to grow with your business and handle increasing claim volumes efficiently.
Every solution is tailored to meet specific business requirements, ensuring better integration and usability.
PixelBrainy ensures long-term success through continuous monitoring and improvement of the system.
Problem: A healthcare provider was struggling with slow claim approvals, high manual workload, and frequent claim rejections due to errors.
Solution: PixelBrainy developed a customized AI Medical Claims Processing Automation Software that automated the entire claims workflow.
Outcome:
The implementation delivered measurable improvements in operations:
With the right AI development company, building an AI Medical Claims Processing Automation Software becomes faster, more efficient, and aligned with long-term business success.

From understanding the fundamentals to exploring architecture, features, costs, and development steps, it is clear that AI Medical Claims Processing Automation Software is transforming how healthcare claims are managed. By leveraging AI technologies such as machine learning, NLP, and automation, businesses can significantly improve accuracy, reduce processing time, and lower operational costs.
As claim volumes continue to grow, investing in AI medical claims processing software development is no longer optional but a strategic necessity for healthcare providers and insurers aiming to stay competitive. A well-designed solution not only enhances efficiency but also ensures scalability and compliance in complex healthcare environments.
Choosing the right technology partner plays a crucial role in success.
Ready to build your AI Medical Claims Processing Automation Software? Book an appointment today and take the first step toward smarter, faster, and more efficient claims processing.
AI solves complex problems such as handling unstructured medical data, detecting hidden fraud patterns, and enabling real-time decision-making. Unlike traditional systems, it continuously learns from data and improves accuracy over time.
Yes, small healthcare providers can benefit by reducing manual workload, minimizing claim errors, and improving cash flow. Even basic AI solutions can significantly improve efficiency and reduce operational costs.
The implementation timeline depends on complexity, but typically ranges from 2 to 12 months. Basic systems can be deployed quickly, while advanced enterprise solutions require more time for development and integration.
AI models require historical claims data, medical records, billing information, and insurance policy data. Clean and well-structured data improves model accuracy and system performance.
Yes, modern AI systems are designed to integrate with existing hospital management systems, EHR platforms, and insurance software using APIs. This ensures seamless data flow and minimal disruption.
AI systems are built with strong security measures such as data encryption, access control, and compliance with healthcare regulations. This ensures that sensitive patient and claims data remains protected.
The future includes real-time claims adjudication, predictive analytics, and more advanced automation. AI will continue to improve efficiency, reduce fraud, and enhance decision-making in healthcare insurance systems.
About The Author
Sagar Bhatnagar
Sagar Sahay Bhatnagar brings over a decade of IT industry experience to his role as Marketing Head at PixelBrainy. He's known for his knack in devising creative marketing strategies that boost brand visibility and market influence. Sagar's strategic thinking, coupled with his innovative vision and focus on results, sets him apart. His track record of successful campaigns proves his ability to utilize digital platforms effectively for impactful marketing efforts. With a genuine passion for both technology and marketing, Sagar continuously pushes PixelBrainy's marketing initiatives to greater success.


Transform your ideas into reality with us.
Working with the PixelBrainy team has been a highly positive experience. They understand the design requirements and create beautiful UX elements to meet the application needs. The dev team did an excellent job bringing my vision to life. We discussed usability and flow. Sagar worked with his team to design the database and begin coding. Working with Sagar was easy. He has the knowledge to create robust apps, including multi-language support, Google and Apple ID login options, Ad-enabled integrations, Stripe payment processing, and a Web Admin site for maintaining support data. I'm extremely satisfied with the services provided, the quality of the final product, and the professionalism of the entire process. I highly recommend them for Android and iOS Mobile Application Design and Development.

Great experience working with them. Had a lot of feedback and I found that unlike most contractors they were bugging me for updates instead of the other way around. They were extremely time conscience and great at communicating! All work was done extremely high quality and if not on time, early! They were always proactive when it comes to communication and the work is great/above par always. Very flexible and a great team to work with! Goes above and beyond to present us with multiple options and always provides quality. Amazing work per usual with Chitra. If you have UI/UX or branding design needs I recommend you go to them! Will likely work with them in the future as well, definitely recommended!

PixelBrainy is a joy to work with and is a great partner when thinking through branding, logo, and website layout. I appreciate that they spend time going into the "why" behind their decisions to help inform me and others about industry best practices and their expertise.

I hired them to design our software apps. Things I really like about them are excellent communication skills, they answer all project suggestions and collaborate right away, and their input on design and colors is amazing. This project was complex and needed patience and creativity. The team is amazing to do business with. I will be using them long-term. Glad to see there are some good people out there. I was afraid to try and outsource my project to someone but I am glad I met them! I really can't say enough. They went above and beyond on this project. I am very happy with everything they have done to make my business stand out from the competition.

It was great working with PixelBrainy and the team. They were very responsive and really owned the project. We'll definitely work with them again!

I recently worked with the PixelBrainy team on a project and I was blown away by their communication skills. They were prompt, clear, and articulate in all of our interactions. They listened and provided valuable feedback and suggestions to help make the project a success. They also kept me updated throughout the entire process, which made the experience stress-free and enjoyable.

PixelBrainy is very good at what it does. The team also presents themselves very professionally and takes care of their side of things very well. I could fully trust them taking up the design work in a timely and organised manner and their attention to detail saved us lots of effort and time. This particular project was quite intense and the team showed that they function very well under pressure. Very much looking forward to working with her again!

It's always an absolute pleasure working with them. They completed all of my requests quickly and followed every note I had for them to a T, which made our process go smoothly from start to finish. Everything was completed fast and following all of the guidelines. And I would recommend their services to anyone. If you need any design work done in the future, PixelBrainy should be your first call!

They took ownership of our requirements and designed and proposed multiple beautiful variants. The team is self-motivated, requires minimum supervision, committed to see-through designs with quality and delivering them on time. We would definitely love to work with PixelBrainy again when we have any requirements.

PixelBrainy was a big help with our SaaS application. We've been hard at work with a new UI/UX and they provided a lot of help with the designs. If you're looking for assistance with your website, software, or mobile application designs, PixelBrainy and the team is a great recommendation.

PixelBrainy designers are amazing. They are responsive, talented, and always willing to help craft the design until it matches your vision. I would recommend them and plan to continue them for my future projects and more!!!

They were awesome! Did a good job fast, and good communication. Will work with them again. Thank you

Creative, detail-oriented, and talented designers who take direction well and implement changes quickly and accurately. They consistently over-delivered for us.

PixelBrainy team is very talented and creative. Great designers and a pleasure to work with. PixelBrainy is an excellent communicator and I look forward to working with them again.

PixelBrainy has a very talented design team. Their work is excellent and they are very responsive. I enjoy working with them and hope to continue on all of our future projects.
